| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Tick Paralysis
🕷️ Note: Tick paralysis most often affects children, presenting as an acute ascending flaccid paralysis. Removal of the engorged tick usually results in rapid and dramatic recovery within 24–48 hours.
🌍 Overview
- Geographic prevalence: Mainly seen in the United States and Australia.
- High-risk group: Children with recent outdoor activities in tick-prone areas.
- Animals affected: Dogs, cats, and cattle are also vulnerable (important in veterinary practice).
- Tick species:
- 🇺🇸 Dermacentor andersoni & Dermacentor variabilis
- 🇦🇺 Ixodes holocyclus
🧬 Pathophysiology
- Tick saliva contains a neurotoxin that blocks acetylcholine release at the neuromuscular junction.
- Toxin effects peak after 5–7 days of attachment → progressive paralysis.
- Distinct from GBS: not immune-mediated, and symptoms reverse quickly once the tick is removed.
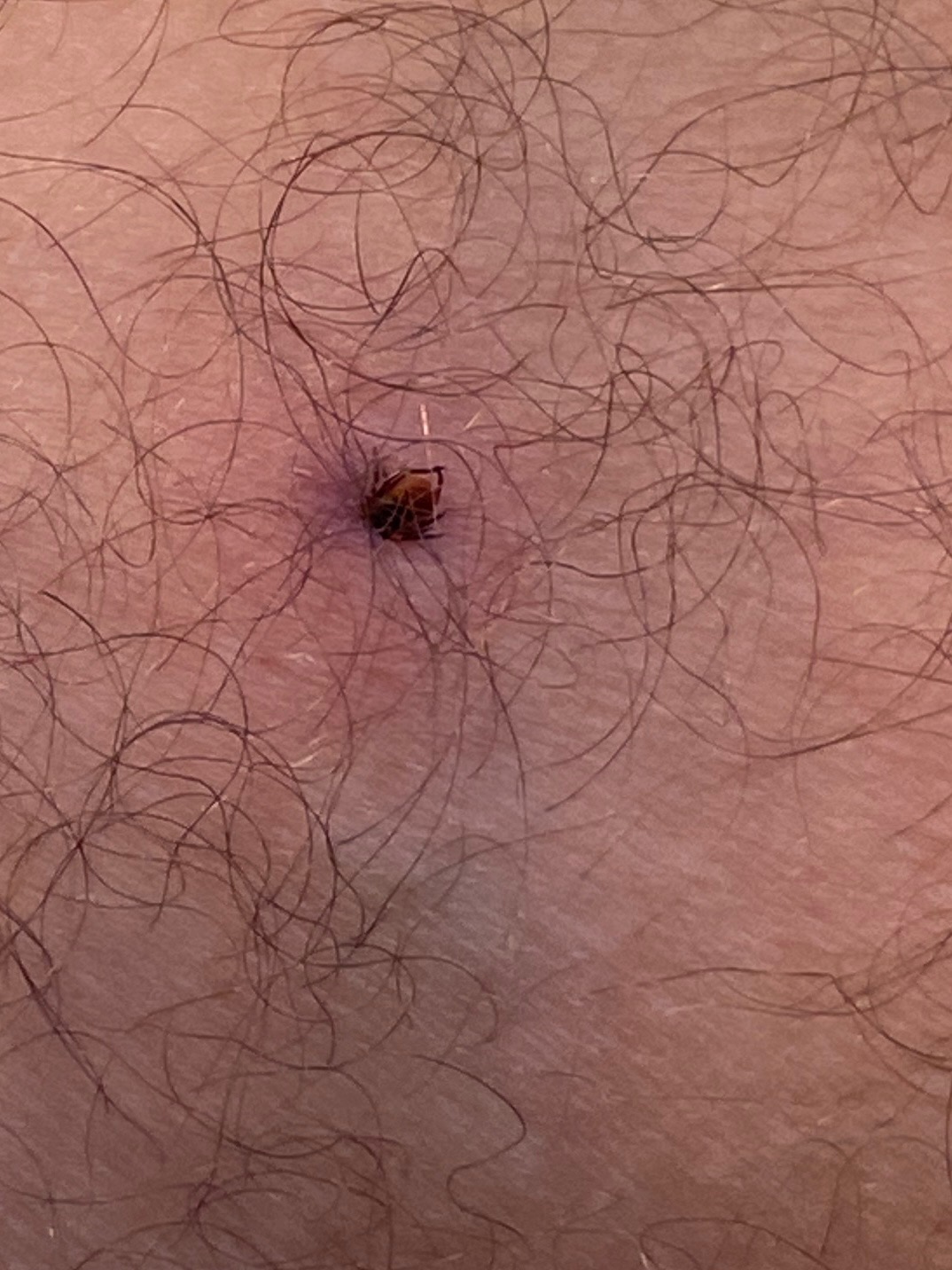
🩺 Clinical Features
- Progressive paralysis: Onset 2–7 days post-attachment → ascending flaccid paralysis.
- Associated symptoms:
- 🌟 Paresthesias, irritability, fatigue, myalgias.
- 🧠 Cranial nerve involvement: facial palsy, bulbar palsy, ophthalmoplegia.
- ⚠️ Severe: respiratory failure, hyporeflexia/areflexia.
- Tick bite location: Often hidden (scalp, nape, skin folds). Thorough examination is essential.
🧾 Differential Diagnosis
- Guillain-Barré Syndrome (GBS): Both cause ascending paralysis, but GBS develops over days–weeks, is immune-mediated, and requires immunotherapy, whereas tick paralysis reverses after tick removal.
🧪 Investigations
- Clinical assessment: Careful skin and scalp inspection to identify tick.
- Electromyography (EMG): May show reduced CMAP amplitude but improves after tick removal.
- Lab tests generally unremarkable → diagnosis is clinical + confirmed by tick detection.
⚕️ Management
- Immediate tick removal: Use fine-tipped tweezers, grasp close to skin, pull steadily upward. ❌ Do not crush or burn the tick.
- Monitoring and supportive care:
- Watch closely for respiratory compromise; ventilation if needed.
- Hydration, analgesia, reassurance for child and family.
- Prevention:
- 👕 Wear long sleeves/pants in tick-prone areas.
- 🦟 Use repellents (DEET or permethrin-treated clothing).
- 🔍 Full-body tick checks after outdoor activities.
📌 Key Takeaways
- 🕷️ Tick paralysis = rare, reversible cause of acute flaccid paralysis.
- ⏱️ Early tick detection and removal → rapid recovery, often within 24 hours.
- ❗ Always consider in children with acute paralysis + outdoor exposure, to avoid misdiagnosis as GBS.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
