| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Fabry disease
Related Subjects: |Autosomal Dominant |Autosomal Recessive |X Linked Recessive |Osteoporosis
🧬 Fabry disease is a rare X-linked lysosomal storage disorder caused by deficiency of the enzyme α-galactosidase A. This leads to pathological accumulation of globotriaosylceramide (GL-3 or Gb3) in multiple organs. The result is a multi-systemic disease with dermatological, renal, neurological, ocular, and cardiovascular involvement. Without treatment, progressive organ failure shortens life expectancy.
📖 About
- Inherited in an X-linked recessive manner. Males are usually more severely affected, but heterozygous females can also show symptoms due to random X-inactivation (lyonisation).
- Incidence: ~1 in 40,000 males 👶, though newborn screening suggests higher prevalence of late-onset variants.
- One of the few lysosomal storage diseases for which enzyme replacement therapy (ERT) is available.
- Classic Fabry disease often presents in childhood; late-onset forms may present only with cardiac or renal disease in adulthood.
🧬 Aetiology & Pathophysiology
- Mutations in the GLA gene (Xq22.1) → deficiency of α-galactosidase A enzyme.
- Accumulation of GL-3 in lysosomes of vascular endothelial cells, smooth muscle, renal epithelial cells, and cardiac myocytes → progressive cellular dysfunction.
- Vascular GL-3 deposition → impaired blood flow, inflammation, and fibrosis → multi-organ complications (stroke, cardiomyopathy, renal failure).
- Blood group B individuals may be more severely affected since α-GAL A also helps break down B antigens.
🌈 Clinical Features
- Skin 🟤: Angiokeratomas (tiny, dark red-purple skin lesions), classically in a "bathing trunk" distribution (between knees and umbilicus).
- Neurological ⚡: Pain crises (acroparaesthesiae) with burning pain in hands/feet, especially in childhood; risk of early strokes (often posterior circulation).
- Renal 💧: Proteinuria, polyuria, progressive CKD; may progress to ESRD. Fanconi-like tubular dysfunction possible.
- Cardiac ❤️: LVH, arrhythmias, heart failure, valvular disease → major cause of death in late-onset forms.
- Ocular 👁️: Cornea verticillata (whorled corneal deposits), lens opacities, vascular tortuosity.
- Other: Hypohidrosis (↓ sweating), heat intolerance, lymphoedema, osteoporosis, GI symptoms (diarrhoea, abdominal pain).
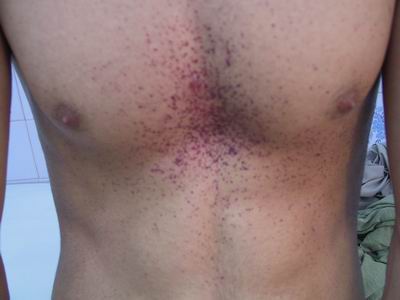
Fabry disease: GL-3 accumulation causes systemic involvement
🔍 Investigations
- Enzyme Assay 🧪: Low α-galactosidase A activity in leukocytes, plasma, or dried blood spot confirms diagnosis in males.
- Genetic Testing 🧬: Identifies GLA mutation; crucial for confirming carrier status in females.
- Urine Analysis: Proteinuria + elevated GL-3.
- MRI Brain 🧠: May show white matter lesions and pulvinar sign (posterior thalamic calcification).
- Cardiac Work-up: ECG/echo for LVH, arrhythmias; cardiac MRI can show late gadolinium enhancement (fibrosis).
- Renal Biopsy: Zebra bodies on EM; reserved for atypical cases.
- Ophthalmology 👁️: Slit-lamp reveals cornea verticillata.
- Prenatal Diagnosis: Enzyme assay in amniocytes or chorionic villus sampling.
💊 Management
- Enzyme Replacement Therapy (ERT) 💉: Recombinant α-galactosidase A (agalsidase alfa or beta) slows GL-3 accumulation and organ damage.
- Chaperone Therapy 💊: Migalastat stabilises certain mutant enzymes (only in amenable mutations).
- Renal Care 💧: ACE inhibitors/ARBs for proteinuria, dialysis or renal transplantation for ESRD.
- Cardiac Care ❤️: Arrhythmia monitoring, pacemakers, heart failure therapy, cardiac MRI surveillance.
- Pain Control ⚡: Neuropathic agents (gabapentin, carbamazepine, TCAs).
- Supportive: Physical therapy, psychological support, patient education, and genetic counselling for families.
📌 Clinical Pearls
- Classic male Fabry = angiokeratomas + neuropathic pain + corneal verticillata + renal dysfunction.
- Females can be anything from asymptomatic carriers to as severe as males.
- Always consider in young patients with stroke (esp. posterior circulation, LVH, proteinuria).
- ERT works best when started before irreversible organ damage has occurred.
📚 References
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
