| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Primary amoebic meningoencephalitis (PAM)
🧠 Naegleria fowleri (“brain-eating amoeba”) is rare but almost universally fatal. Most infections occur in young males, especially ≤14 years old. Mortality exceeds 95%, making early recognition and prevention critical.
🌍 About
- Causes a rapidly progressive brain infection in children and adolescents.
- Leads to severe cerebral swelling and herniation.
- Less common in chlorinated or salt water (chlorination protective).
🦠 Aetiology
- Naegleria fowleri – a free-living thermophilic amoeba.
- Found in warm fresh water 💧 (lakes, rivers, hot springs) and soil.
- Risk in unchlorinated swimming pools 🏊♂️.
- Enters via the nose → olfactory nerves → cribriform plate → brain.
- Usually linked to swimming, diving, or water sports with head submersion.
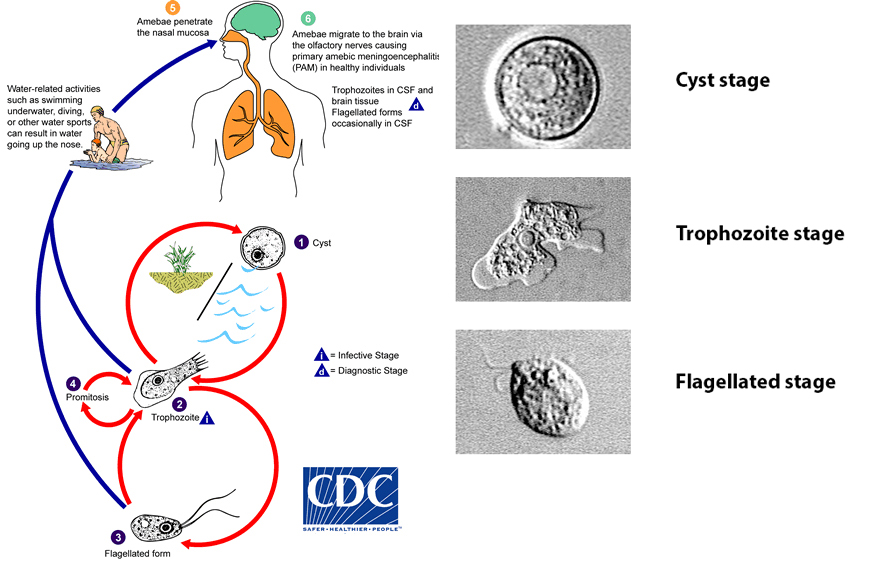
⚠️ Clinical
- Onset usually within 1 week of exposure.
- Initial: headache, fever, nausea, vomiting 🤒.
- Meningism: stiff neck, photophobia, confusion.
- Progression: seizures, hallucinations, coma → death.
🔎 Investigations
- FBC, U&E, LFTs: usually unremarkable.
- CT/MRI: cerebral swelling, oedema, haemorrhage.
- CSF (if safe): often grey–red, high RBCs, neutrophilic pleocytosis (>28,000 WCC), ↑ protein, trophozoites may be seen on wet mount. 🚨 Often avoided due to raised ICP.
💊 Management
- Mortality >95%; only ~10 documented survivors worldwide 🌍.
- Supportive: ABC, resuscitation, ICP management.
- Often misdiagnosed and treated empirically as bacterial meningitis.
- Antimicrobials tried: Amphotericin B (IV + intrathecal), Azithromycin, Fluconazole, Rifampin, Miltefosine, Dexamethasone.
- Early aggressive combination therapy + ICP management offers the best (but still slim) chance of survival.
📚 References
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
