| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Tests in Liver Disease: Usefulness and Interpretation
Related Subjects: |Chronic liver disease |Cirrhosis |Alkaline phosphatase (ALP) |Liver Function Tests |Ascites Assessment and Management |Budd-Chiari syndrome |Autoimmune Hepatitis |Primary Biliary Cirrhosis |Primary Sclerosing Cholangitis |Wilson disease |Hereditary Haemochromatosis |Alpha-1 Antitrypsin (AAT) deficiency |Non alcoholic steatohepatitis (NASH) |Spontaneous Bacterial Peritonitis |Alcoholism and Alcoholic Liver Disease
⚠️ These are not true “liver function tests” but rather markers of liver damage or cholestasis. 👉 Normal LFTs ≠ normal liver. 🚨 The three main causes of severe derangement of all enzymes are: Hepatic ischaemia, Viral hepatitis, and Drugs/Toxins.
🧪 Key Liver Blood Tests
- 🔴 AST (Aspartate Aminotransferase) – Raised in liver injury (esp. alcohol-related) but not liver-specific. Also elevated in heart and muscle disease.
- 🟠 ALT (Alanine Aminotransferase) – More specific to hepatocyte injury (e.g. viral hepatitis, NAFLD).
- 🟡 ALP (Alkaline Phosphatase) – Marker of cholestasis or obstruction. Also made in bone & placenta ➡️ check GGT to confirm hepatic origin.
- 🟢 GGT (Gamma-Glutamyl Transferase) – Rises with ALP in biliary disease. Sensitive to alcohol and drugs (phenytoin, barbiturates).
- 💛 Bilirubin – Breakdown product of haem. – Conjugated ↑ → obstruction, hepatocellular disease – Unconjugated ↑ → haemolysis, Gilbert’s syndrome.
- 💙 Albumin – Low in chronic liver disease (ascites, oedema). Also reduced in nephrotic syndrome, sepsis, malnutrition.
- 🩸 PT/INR – Prolonged if liver fails to make clotting factors. Important in paracetamol overdose & acute liver failure. Always give Vit K to exclude deficiency.
- 🟣 Platelets – Low in cirrhosis due to splenomegaly & portal hypertension.
- 🧬 AFP (Alpha-Fetoprotein) – Tumour marker for hepatocellular carcinoma (HCC).
- ☁️ Ammonia – Raised in hepatic encephalopathy (toxic accumulation).
- 🔍 Liver Biopsy – Gold standard for diagnosis & staging fibrosis (can be via jugular if coagulopathy).
- 📡 FibroScan – Non-invasive measure of stiffness (fibrosis/cirrhosis).
- 🖼️ Imaging (USS, CT, MRI) – Liver size, morphology, masses, biliary tree, ascites, vascular flow.
📖 Focused History for Abnormal LFTs
- 💊 Medications – recent antibiotics, herbal remedies, paracetamol use.
- 🌍 Travel – rural/countryside, water sports (e.g. leptospirosis).
- 💉 IV or recreational drug use (Hep B/C risk).
- 🍺 Alcohol intake – CAGE questions, history of withdrawal (DTs).
- ❤️ Sexual history & transfusions pre-1990 (HIV, Hepatitis risk).
- 🤒 Associated symptoms – fever, rigors, vomiting, pale stools, dark urine, pruritus, weight loss, abdo pain.
- 🔎 Features of chronic liver disease – ascites, encephalopathy, coagulopathy, jaundice.
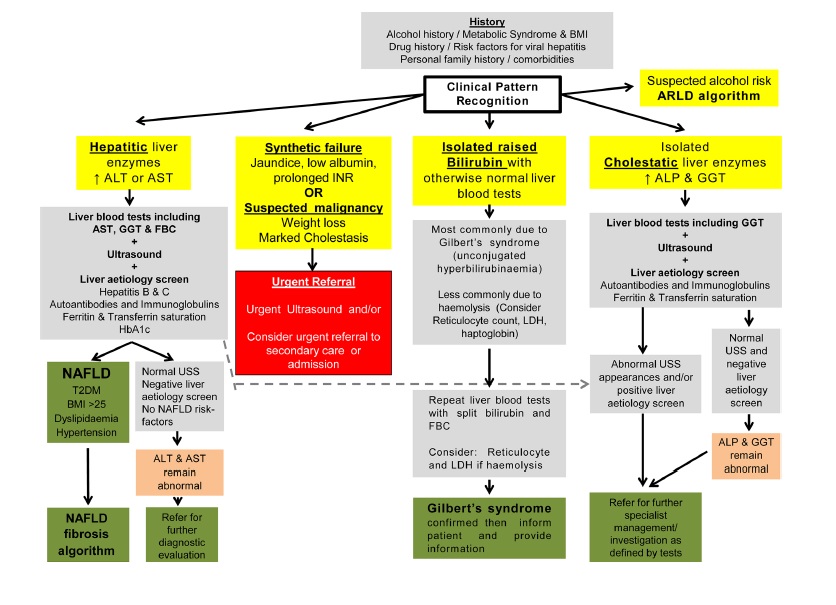
🚨 Causes of Liver Injury
- 🦠 Viral hepatitis (A–E, CMV, EBV, HSV).
- 🍺 Alcohol-related liver disease.
- 💊 Drug-induced hepatotoxicity (paracetamol, statins, anti-TB meds).
- 💔 Ischaemic hepatitis (“shock liver”).
- 🟢 Obstructive jaundice (stones, tumours, PSC/PBC).
- ⚖️ NAFLD with T2DM (AST > ALT pattern).
🧾 Interpretation of Specific Tests
- 🩸 PT/INR – Reflects liver synthetic function. Raised in paracetamol OD, fulminant failure. Always try Vit K → persistent abnormality = true liver dysfunction.
- 💙 Albumin – Falls in cirrhosis, but also sepsis, nephrotic syndrome, malnutrition.
- 💧 Urea – Often low in liver disease (reduced metabolism). High in GI bleed (protein load).
- ☁️ Ammonia – Linked to encephalopathy, esp. fulminant liver failure.
- 🟡 Bilirubin – Conjugated ↑ = obstruction; Unconjugated ↑ = haemolysis, Gilbert’s.
- 🟡 ALP – Canalicular enzyme, cholestasis. Cross-check with GGT.
- 🟠 AST/ALT – – AST:ALT > 2 → Alcoholic liver disease 🍺 – ALT more specific to liver 🧡 – Mild ↑ (<100): chronic hepatitis, fatty liver – Moderate ↑ (100–300): autoimmune hepatitis, NASH, Wilson’s – Marked ↑ (>300): paracetamol OD, viral hepatitis, ischaemia.
🧪 Further Investigations (“Liver Screen”)
- 🦠 Viral serology – HBsAg, HCV Ab, HAV IgM, HSV, CMV, HIV, ± Hepatitis D IgM.
- 🧬 Autoimmune markers – ANA, ASMA, AMA, immunoglobulins.
- ⚖️ Metabolic – Ferritin, transferrin saturation, caeruloplasmin & copper (if <55), A1AT phenotype.
- 🩸 AFP – screen for HCC.
- 🩺 Imaging – USS (structure, obstruction, PV patency), MRCP/ERCP if obstructive pattern.
- 💉 Biopsy – histology & fibrosis staging.
- 🚨 NAC early if any suspicion of paracetamol overdose.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
