| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Coeliac disease ✅
Related Subjects: |Colorectal cancer |Colorectal polyps |Ulcerative Colitis |Acute Severe Colitis |Crohn's disease |Coeliac disease
⚠️ Coeliac disease carries an increased risk of malignancy (especially enteropathy-associated T-cell lymphoma, small bowel adenocarcinoma, and squamous cell carcinoma of the oropharynx/oesophagus). 👉 New or unexplained symptoms in a diagnosed patient should always prompt review, as they may indicate complications or malignant transformation.
ℹ️ About
- Coeliac disease is a chronic autoimmune enteropathy triggered by dietary gluten (found in wheat, rye, barley).
- Prevalence ≈ 1 in 100 in Western populations; in the UK, incidence ≈ 1 in 2000, highest in western Ireland (≈ 1 in 300).
- Can present at any age – adults with new GI or systemic symptoms should be considered for testing.
🧬 Aetiology & Pathophysiology
- Immune reaction to α-gliadin → T-cell mediated release of interferon-γ → villous atrophy, crypt hyperplasia, and lymphocytic infiltration.
- Strong genetic predisposition: 95% carry HLA-DQ2 or HLA-DQ8.
- Associated autoimmune conditions: type 1 diabetes, autoimmune thyroid disease, autoimmune liver disease.
🧒 Clinical Features
- Infants/young children: Failure to thrive, abdominal distension, abnormal stools, anaemia, irritability.
- Older children/adults: Fatigue, diarrhoea, steatorrhoea, abdominal pain, weight loss, headaches, arthralgia.
- Extra-intestinal features: Iron/folate deficiency anaemia, osteoporosis/osteomalacia, infertility, neurological manifestations (peripheral neuropathy, ataxia).
- Dermatitis herpetiformis: Intensely itchy rash on elbows, knees, and buttocks; pathognomonic for coeliac disease.
🧪 Investigations
- Blood tests: FBC, iron/folate/vitamin B12, calcium, phosphate, ALP, albumin, PT/INR. Howell–Jolly bodies may indicate hyposplenism.
- Serology: IgA anti-tTG (first-line, high sensitivity/specificity), total IgA to rule out IgA deficiency, anti-endomysial antibodies if needed.
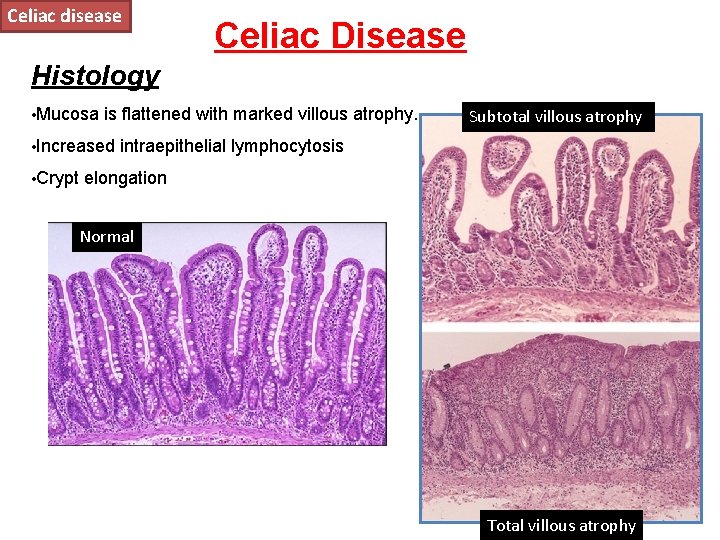
- Endoscopy + biopsy: Multiple duodenal biopsies show villous atrophy, crypt hyperplasia, and intraepithelial lymphocytosis (gold standard).
🔍 Differentials
- Tropical sprue, cystic fibrosis, milk protein enteropathy.
- Infective: Giardiasis.
- Other: chronic pancreatitis, abetalipoproteinaemia.
💊 Management
- Gluten-free diet (GFD): Lifelong adherence is cornerstone. Monitor antibody titres for adherence.
- Nutritional supplementation: Iron, folate, calcium, vitamin D, and fat-soluble vitamins as required.
- Refractory cases: Short course of corticosteroids or immunosuppressants if strict GFD fails.
- Family screening: First-degree relatives should be considered for testing.
- Follow-up: Monitor growth in children, bone health, antibody titres, and symptoms; re-biopsy only if symptoms persist.
⚠️ Complications
- Growth retardation and delayed puberty in children.
- Osteopenia, osteoporosis, and osteomalacia due to malabsorption.
- Malignancy: enteropathy-associated T-cell lymphoma, small bowel adenocarcinoma, oesophageal SCC.
- Hyposplenism → risk of overwhelming sepsis (vaccinate against encapsulated organisms).
📌 Key Teaching Points
- Always test for coeliac disease before diagnosing IBS in adults.
- Do not start a gluten-free diet before biopsy confirmation – can normalize histology and obscure diagnosis.
- Vaccinate against pneumococcus if hyposplenic.
- Long-term follow-up essential: monitor nutrition, bone density, and malignancy risk.
Cases – Coeliac Disease
- Case 1 (Classic pediatric): 9-year-old boy with chronic diarrhoea, abdominal distension, faltering growth, iron-deficiency anaemia, low vitamin D. Anti-tTG IgA raised; duodenal biopsy confirms villous atrophy. Management: Lifelong GFD, dietitian support, iron & vitamin D supplementation. Outcome: Growth improves, anaemia resolves, antibody titres fall.
- Case 2 (Atypical adult): 42-year-old woman with fatigue, aphthous ulcers, refractory iron-deficiency anaemia, no GI symptoms. Anti-tTG positive; biopsy confirms coeliac disease. Management: Gluten-free diet, nutrition counselling, iron replacement. Outcome: Symptom improvement and normal Hb after 4 months.
- Case 3 (Silent/subclinical): 55-year-old man with osteoporosis after low-impact fracture, mild anaemia, elevated anti-tTG, villous blunting on biopsy. Management: Gluten-free diet, calcium & vitamin D, bisphosphonate therapy. Outcome: Bone density stabilises, anaemia improves, patient educated on strict diet adherence.
Teaching Commentary 🧑⚕️
These cases illustrate the spectrum of coeliac disease:
1) Classic malabsorptive form in children.
2) Atypical/extra-intestinal presentation in adults.
3) Silent/subclinical disease detected through complications like osteoporosis.
The disease is immune-mediated, triggered by gluten peptides, leading to villous atrophy. Management is always a lifelong gluten-free diet with dietitian support. Monitor for deficiencies, bone health, and malignancy risk. Early recognition prevents irreversible complications.
📚 References
- NICE Guideline: Coeliac Disease – Recognition, Assessment and Management (NG20)
- Coeliac UK – Information & Resources
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
