| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Farmer's lung
Related Subjects: |Idiopathic Pulmonary Fibrosis |Diffuse Parenchymal Lung disease |Asbestos Related Lung disease |Sarcoidosis |Coal Worker's Pneumoconiosis |Silicosis |Farmer's Lung |Cryptogenic Organising Pneumonia (COP-BOOP) |Extrinsic Allergic alveolitis (Hypersensitivity) |Pneumoconiosis |Cor Pulmonale
🌾 Farmer’s Lung (a form of Hypersensitivity Pneumonitis / Extrinsic Allergic Alveolitis) is an immune-mediated reaction to inhaled organic antigens. ⚠️ The spores are not infectious - the disease is allergic in origin. 🐦 Bird Fancier’s Lung usually carries a worse prognosis than Farmer’s Lung.
📖 About
- An allergic reaction to inhaled antigens rather than an infection.
- One of the most common occupational interstitial lung diseases in the UK.
- Triggered by microbes (esp. Saccharopolyspora rectivirgula) growing on mouldy hay and crops.
🧪 Aetiology
- Exposure to mouldy hay, straw, or grain (especially in damp, poorly ventilated barns).
- Pesticides (organochlorines, carbamates) may increase susceptibility.
- Moisture + heat → microbial growth → spore release.
🩺 Clinical Features
- Acute: 4–8 hrs post-exposure → dyspnoea, dry cough, fever, chills, malaise, tachycardia.
- Subacute: Ongoing low-level exposure → chronic cough, breathlessness, arthralgia, weight loss.
- Chronic: Years of exposure → progressive dyspnoea, cyanosis, digital clubbing, irreversible fibrosis.
🔍 Investigations
- Bloods: FBC usually normal; CRP/ESR may be ↑.
- Serology: Antigen-specific IgG = supportive evidence.
- PFTs: Restrictive in acute/subacute; mixed restrictive/obstructive in chronic.
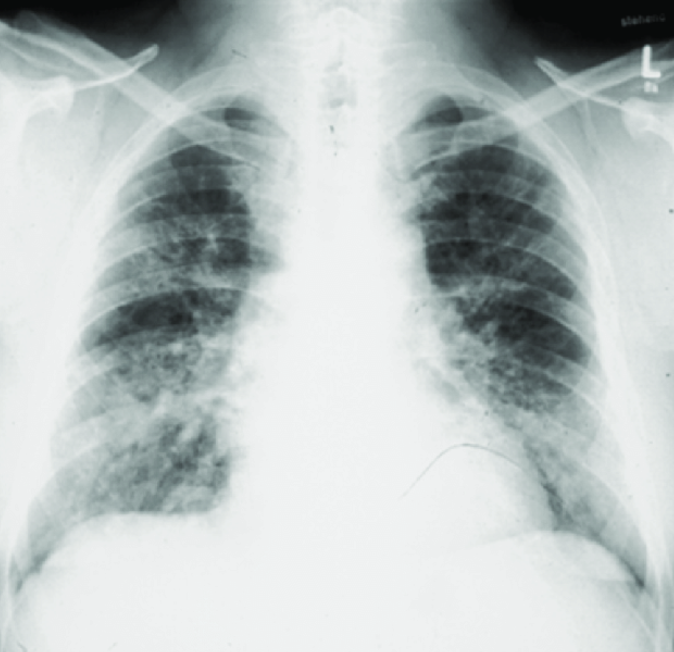
- CXR: Diffuse micronodular shadowing (mid/upper zones). Chronic → fibrosis, volume loss.
- HRCT: Ground-glass opacities, centrilobular nodules, air-trapping; fibrosis in chronic disease.
- BAL: Lymphocytosis with ↓ CD4/CD8 ratio (<1.0).
- Biopsy: Interstitial inflammation ± fibrosis (UIP pattern if advanced).
⚠️ Complications
- Progressive pulmonary fibrosis.
- Respiratory failure (type 1 hypoxaemia).
- Pulmonary hypertension and cor pulmonale.
- Chronic disability if exposure continues.
💊 Management
- Acute: O₂ for hypoxaemia, corticosteroids (prednisolone) in severe cases.
- Chronic/Resistant: Consider steroid-sparing agents (azathioprine, mycophenolate).
- Exposure Control:
- Dry crops thoroughly before storage.
- Maintain good barn ventilation.
- Use protective masks/respirators.
- Prognosis: Early recognition and avoidance of antigen = best outcome.
📚 References
3 Clinical Cases - Farmer’s Lung 🌾🫁
- Case 1 - Acute exposure 🌬️: A 45-year-old dairy farmer develops fever, chills, dry cough, and dyspnoea 6 hours after handling mouldy hay. CXR shows diffuse patchy infiltrates. Symptoms improve on leaving the barn but recur with re-exposure. Teaching: Farmer’s Lung is an acute hypersensitivity pneumonitis due to inhaled thermophilic actinomycetes spores. Acute episodes can mimic pneumonia but improve with antigen avoidance and corticosteroids.
- Case 2 - Subacute presentation 📆: A 52-year-old man presents with weeks of progressive breathlessness and weight loss. HRCT shows ground-glass opacities and centrilobular nodules. Bloods: raised ESR, precipitating antibodies to Saccharopolyspora rectivirgula. Teaching: Subacute Farmer’s Lung presents with insidious symptoms, often misdiagnosed as viral or atypical pneumonia. Diagnosis rests on exposure history, radiology, and immunology. Management is strict antigen avoidance + steroids if persistent.
- Case 3 - Chronic fibrotic disease 🧑🌾: A 60-year-old lifelong farmer has longstanding cough and progressive exertional dyspnoea. HRCT: upper lobe fibrosis, honeycombing, and traction bronchiectasis. PFT: restrictive pattern with reduced DLCO. Teaching: Chronic Farmer’s Lung leads to irreversible interstitial fibrosis if untreated. Prognosis worsens with continued exposure. Early recognition is key - chronic disease may resemble idiopathic pulmonary fibrosis.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
