| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Neck Swellings by Triangle
Related Subjects: |Neck Swellings by Triangle |Thyroglossal cyst |Head and Neck Cancers |Triangles of the neck
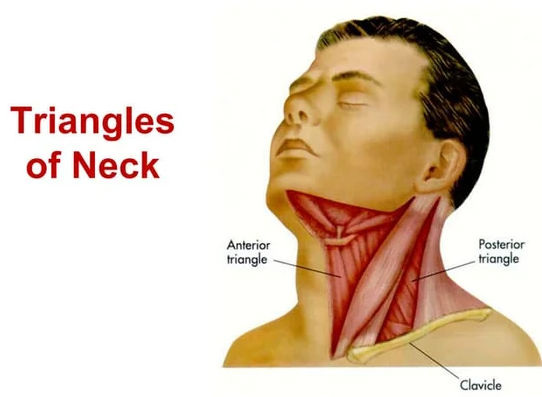
🩺 Neck Swellings - Anterior Triangle & Midline (Corrected & Structured)
Neck lumps are common in clinical practice. In adults, a persistent neck lump (>3 weeks) is malignancy until proven otherwise ⚠️. Anatomical location (anterior triangle vs midline), movement with swallowing, and movement with tongue protrusion are key diagnostic clues.
🧾 Key Pathologies
| Pathology | Clinical Presentation & Key Features 🩺 | Diagnosis & Management 🔎💊 |
|---|---|---|
| Thyroglossal Duct Cyst 👅 |
|
Diagnosis:
• Ultrasound first-line (cystic, relation to hyoid/thyroid) • Confirm normal thyroid gland present (avoid excising only functioning thyroid) • TFTs + thyroid US • FNAC if solid areas or adult presentation • CT/MRI for complex/tract delineation Management: • Antibiotics + drainage if infected/abscess • Definitive: Sistrunk procedure (cyst + midline tract + central hyoid resection) • Recurrence ~5–10% (much higher without hyoid removal) • Postoperative TFT monitoring if ectopic thyroid suspected |
| Branchial Cyst (2nd arch most common) 💧 |
|
Diagnosis:
• Ultrasound ± FNAC (squamous debris, cholesterol crystals) • CT/MRI to delineate tract & deep extension • Adults: panendoscopy + tonsillectomy/biopsy to rule out primary SCC Management: • Treat acute infection first (antibiotics, aspiration if tense) • Complete surgical excision of cyst + tract once inflammation settled • Recurrence 10–20% if incomplete removal |
| Cystic Hygroma (Lymphangioma) 🌟 |
|
Diagnosis:
• Ultrasound: multiloculated cystic mass ± septations • MRI best for extent & deep/compartmental involvement Management: • Observation for small asymptomatic lesions • Sclerotherapy (OK-432, doxycycline, bleomycin) first-line for macrocystic • Surgical debulking/excision for symptomatic or failed sclerotherapy • High recurrence rate (20–50%) |
| Thyroid Goitre / Nodule 🦋 |
|
Diagnosis:
• TFTs (TSH first) • Ultrasound + TI-RADS classification • FNAC (Bethesda I–VI system) • Scintigraphy for hyperfunctioning nodules Management: • Benign/low-risk: surveillance US • Compressive/suspicious: hemithyroidectomy or total thyroidectomy • Toxic nodule/MNG: radioiodine or surgery • Levothyroxine suppression controversial |
| Thyroid Cancer 🎗️ |
|
Diagnosis:
• US + FNAC • Calcitonin/CEA if medullary suspected • CT/MRI/PET for staging Management: • Total thyroidectomy ± central/lateral neck dissection • Radioiodine ablation (differentiated) • TSH suppression lifelong • TKIs (lenvatinib, sorafenib) for advanced |
| Lymphadenopathy 🧬 |
|
Diagnosis:
• FBC, ESR/CRP, LDH • US ± FNAC/core biopsy • Excisional biopsy if lymphoma suspected • CXR, Mantoux/IGRA, HIV, EBV serology Management: • Treat underlying cause (antibiotics, ATT for TB) • Oncology/haematology referral if malignant |
| Carotid Body Tumour (Paraganglioma) ⚡ |
|
Diagnosis:
• Duplex US + CT/MR angiography • Functional imaging (Ga-68 DOTATATE, MIBG) • Never biopsy (highly vascular) Management: • Observation for small/asymptomatic • Preoperative embolisation + surgical resection (Shamblin classification) • Genetic testing (SDHx mutations) |
| Parotid Tumour 🦠 |
|
Diagnosis:
• US + FNAC (Milan system) • MRI for deep lobe / perineural spread Management: • Superficial parotidectomy (benign) • Total parotidectomy + neck dissection ± RT (malignant) • Facial nerve monitoring essential |
Note: This is a simplified plain-HTML version without external CSS. Copy-paste into a .html file to view.
