0️⃣ Definitions (set expectations early)
- NSTEMI: symptoms/signs of myocardial ischaemia + rise/fall in troponin (myocardial necrosis) without persistent ST elevation.
- Unstable angina: ischaemic symptoms (often with ECG changes) but troponin not elevated.
- Core goal: stabilise myocardium, prevent thrombus extension, and use risk-based angiography to reduce recurrent MI/death.
1️⃣ Recognition & Immediate Actions (first 10 minutes)
- 🎯 Suspect with chest pain/pressure (or atypical dyspnoea/collapse) especially in older adults, women, diabetes, CKD.
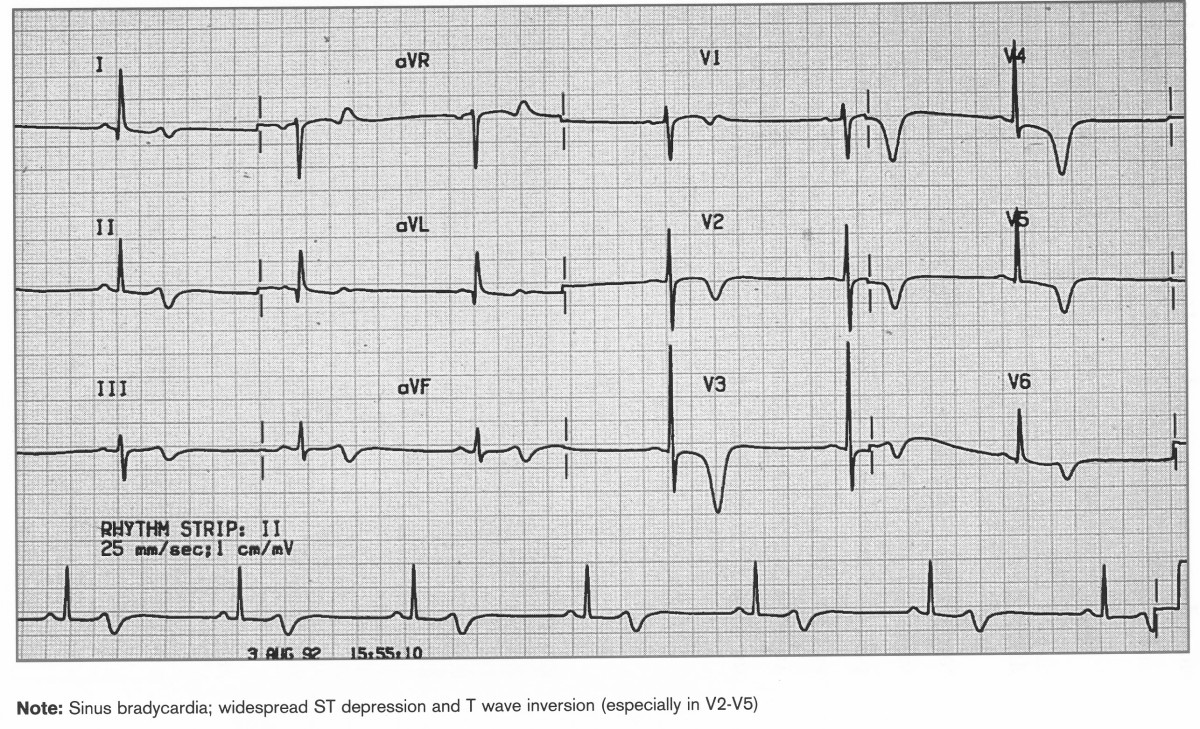
- 📊 12-lead ECG immediately; repeat if pain continues or ECG evolves (e.g., q15–30 min early on).
- 📟 Continuous cardiac monitoring/telemetry; defib available ⚡.
- 🫁 Oxygen only if hypoxaemic (target 94–98%; 88–92% if risk of hypercapnic failure).
- 💉 IV access, baseline obs, NEWS2, point-of-care glucose.
- 🚫 Do not give DAPT before diagnosis is made (avoid bleeding harm in mimics like dissection/PE).
2️⃣ Investigations (do not delay treatment)
- 🧪 Bloods: hs-troponin, FBC, U&E/creatinine, glucose, clotting, LFTs (optional), lipids (can be taken early for baseline).
- ⏱️ Serial troponin: use local hs-troponin pathway (often 0/1–2 h). A dynamic rise/fall supports NSTEMI.
- 📷 CXR if alternative diagnosis suspected (pulmonary oedema, pneumothorax, infection) - do not “routine-delay”.
- 🫀 Echocardiography: assess LV function (all NSTEMI) and look for complications (MR, regional wall motion abnormality, HF).
- 🔎 Consider mimics selectively: dissection (clinical red flags), PE, myocarditis/pericarditis (pleuritic pain, viral prodrome, diffuse ST changes).
3️⃣ Risk Stratification (NICE = GRACE 6-month mortality)
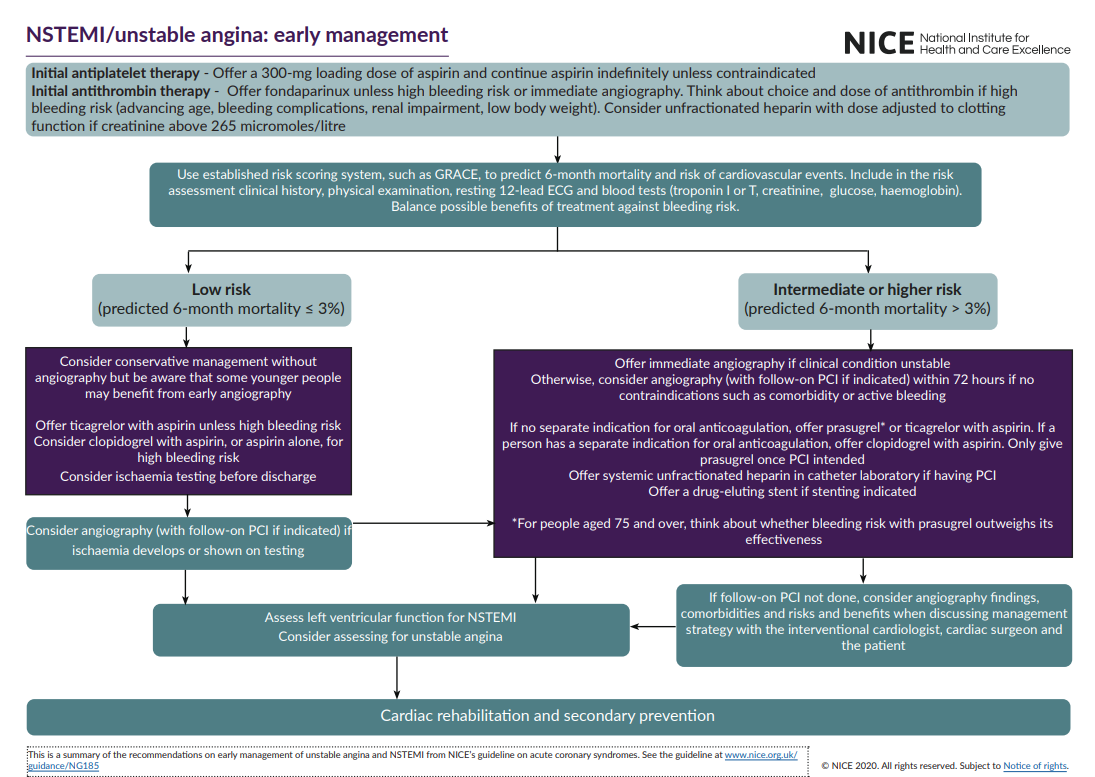
- 📊 Once NSTEMI/UA diagnosis made and aspirin + antithrombin offered, assess risk using a score predicting 6-month mortality (e.g. GRACE).
- 🟢 Low risk: predicted 6-month mortality ≤3% → consider conservative strategy (no early angiography) if clinically stable.
- 🟠 Intermediate/high risk: predicted 6-month mortality >3% → usually benefit from angiography (timing below).
- 🚨 Unstable / very high-risk features: haemodynamic instability, cardiogenic shock, refractory/recurrent ischaemia, malignant arrhythmia (VT/VF), acute HF/pulmonary oedema → immediate angiography.
4️⃣ Immediate Medical Therapy (anti-ischaemic + antithrombotic)
- 💊 Aspirin: 300 mg loading then continue indefinitely unless contraindicated.
- 💉 Antithrombin (NICE):
- Fondaparinux 2.5 mg SC daily unless immediate angiography is planned, or bleeding risk is very high.
- Significant renal impairment (creatinine >265 micromol/L): consider unfractionated heparin (UFH) instead, dose-adjusted to clotting monitoring.
- ⚠️ High bleeding risk: individualise agent/dose (age, prior bleeding, renal impairment, low body weight).
- 🌬️ Nitrates: GTN SL/IV for ongoing ischaemic pain and hypertension if no contraindications (avoid in hypotension, severe AS, suspected RV infarct, recent PDE5 inhibitor).
- 💉 Analgesia: IV opioid titrated to pain + antiemetic if needed.
- 🫀 Beta-blocker: consider early oral beta-blocker if tachycardic/hypertensive and no acute HF/shock/bradycardia/heart block/asthma exacerbation.
- 🧴 High-intensity statin: start early unless contraindicated (dose per local post-ACS pathway).
5️⃣ P2Y12 inhibitor strategy (NICE NG185 - depends on angiography/PCI plan)
- If coronary angiography is planned:
- If no separate indication for ongoing oral anticoagulation: offer prasugrel or ticagrelor with aspirin.
- Prasugrel: only give once coronary anatomy is defined and PCI is intended (and weigh bleeding risk carefully, especially age ≥75).
- If a person does have a separate indication for ongoing oral anticoagulation: offer clopidogrel with aspirin.
- If PCI is not indicated (conservative management):
- Offer ticagrelor + aspirin unless high bleeding risk.
- If high bleeding risk: consider clopidogrel + aspirin or aspirin alone.
6️⃣ Invasive strategy & timing (NICE)
- 🚑 Immediate angiography if clinical condition is unstable (shock, refractory ischaemia, life-threatening arrhythmia, acute HF).
- 🕒 Otherwise, consider angiography (with follow-on PCI if indicated) within 72 hours if no contraindications (e.g., severe comorbidity, active bleeding).
- 🩻 PCI practicals (NICE): if PCI performed, offer systemic UFH in the cath lab whether or not fondaparinux has already been given.
- 🧷 If stenting indicated, offer a drug-eluting stent.
- 🔁 If revascularisation strategy unclear (PCI vs CABG), discuss in a heart-team format (interventional cardiology + cardiac surgery) with the patient.
7️⃣ Supportive care & complication surveillance
- 🛏️ Monitored bed until stable; watch for VT/VF, AF, heart block, recurrent ischaemia.
- 🌊 Treat HF/pulmonary oedema promptly (diuretics, NIV/oxygen if hypoxaemic, specialist input).
- 🧪 Glucose: keep blood glucose <11 mmol/L while avoiding hypoglycaemia; consider dose-adjusted insulin infusion early if needed.
- 🩸 Bleeding prevention: review anticoagulants/NSAIDs, consider gastroprotection if high GI bleed risk (local policy).
- 🧠 Always re-check diagnosis if pain is tearing/back, neuro deficit, pulse deficit, or mediastinal widening → think dissection (avoid antithrombotics until excluded).
8️⃣ Before discharge (NICE)
- 🫀 Assess LV function in all NSTEMI patients and document in discharge summary.
- 🧪 If managed conservatively without angiography: consider ischaemia testing before discharge to quantify inducible ischaemia.
- 📋 Clear plan for antithrombotics, BP, lipids, diabetes control, and follow-up.
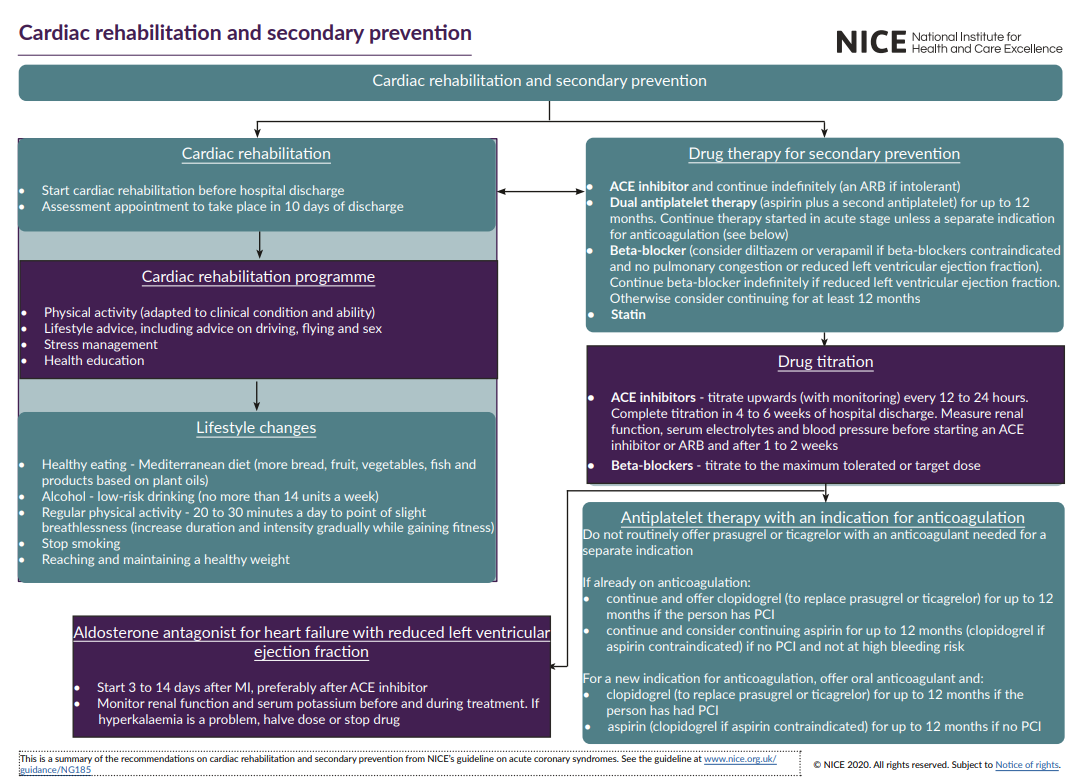
9️⃣ Secondary prevention (long-term survival gains)
- 💊 DAPT: aspirin + selected P2Y12 inhibitor typically for up to 12 months (shorter if bleeding risk high; longer only if specialist-directed).
- 🧴 Statin: high-intensity long-term; consider add-on lipid therapy in very high risk if not at goal (specialist pathway).
- 💊 ACE inhibitor: start once haemodynamically stable and continue indefinitely after MI; titrate to target/max tolerated.
- 🫀 Beta-blocker: especially if LV dysfunction/HF; individualise if preserved EF.
- 🧪 MRA (eplerenone): consider if LVEF ≤40% with HF or diabetes (monitor K+ and renal function).
- 🏥 Cardiac rehabilitation referral + lifestyle: smoking cessation 🚭, Mediterranean diet 🥗, graded exercise 🏃♂️, weight/BP optimisation.
|