| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Thyrotoxicosis and Hyperthyroidism
⚠️ Definitions
- Hyperthyroidism 🔥 = excess production and release of thyroid hormones (T3/T4) from the thyroid.
- Thyrotoxicosis ☢️ = clinical syndrome of thyroid hormone excess, from any source (thyroidal or extrathyroidal).
📊 Prevalence
- 🇪🇺 Europe: ~0.8% of population.
- 🇺🇸 USA: 1–3% prevalence.
- ♀️ More common in women (5–10x higher).
🔎 Causes of Hyperthyroidism / Thyrotoxicosis
- Graves’ disease 🌸 – Commonest cause (esp. women 30–50). – Diffuse goitre, ↑ RAI uptake, ophthalmopathy, pretibial myxoedema. – Autoantibodies: TSH receptor (TRAb). – Smoking 🚬 ↑ risk of eye disease.
- Toxic multinodular goitre 🪢 – Common in older adults, iodine-deficient areas. – Patchy uptake on RAI scan.
- Toxic adenoma (“hot nodule”) 🔥 – Solitary nodule, focal ↑ uptake on scan. – Causes classical thyrotoxicosis.
- Thyroiditis 🦠 – Often post-viral (subacute, painful). – Release of pre-formed hormone (NOT ↑ synthesis). – Features: tender thyroid, ↑ ESR/CRP, ↓ uptake on RAI. – Rx: NSAIDs/β-blockers; steroids if severe.
- TSH-secreting pituitary adenoma 🎯 – Rare. Raised TSH + T4. – Features: thyrotoxicosis + bitemporal hemianopia.
- Hashimoto’s “Hashitoxicosis” 🌀 – Transient thyrotoxic phase in autoimmune thyroiditis. – Antibodies: anti-TPO, anti-TG.
- Jod-Basedow effect 💊 – Thyrotoxicosis after excess iodine (contrast, amiodarone).
- hCG-mediated 🤰 – Hydatidiform mole, choriocarcinoma.
- McCune-Albright syndrome 🧬 – Triad: fibrous dysplasia of bone, café-au-lait spots, endocrine hyperfunction (incl. thyroid).
📊 Comparison Table – Common Causes of Thyrotoxicosis
| Feature | 🌸 Graves’ Disease | 🪢 Toxic Multinodular Goitre (TMNG) | 🔥 Thyroiditis |
|---|---|---|---|
| 👩 Typical Patient | Young–middle aged female (30–50), autoimmune background, smoker 🚬 | Older adults, long-standing goitre, iodine-deficient areas 🌍 | Any age; post-viral (subacute), postpartum, or drug-induced 💊 |
| 🩺 Clinical Features | Diffuse goitre, bruit, ophthalmopathy 👁️, pretibial myxoedema | Nodular, irregular goitre; no eye disease | Painful/tender thyroid (subacute) OR painless (silent, postpartum) |
| 🔬 TFTs | ↑ Free T4/T3, ↓ TSH | ↑ Free T4/T3, ↓ TSH | Early: ↑ T4/T3, ↓ TSH → Later: hypothyroid, then recovery |
| 🧪 Antibodies | +ve TRAb (TSH receptor antibodies) ✅ | Usually negative | Anti-TPO ± Anti-TG (autoimmune forms) |
| 📻 Radioiodine Uptake Scan | Diffuse, homogenous ↑ uptake | Patchy/multiple “hot spots” 🔥 | ↓ Uptake (due to hormone release, not overproduction) |
| 🩻 Imaging | Doppler: ↑ vascularity (“thyroid inferno”) 🔥 | Irregular nodules on USS | Low uptake; USS may show hypoechoic areas |
| 💊 First-Line Treatment | Carbimazole / PTU; ± RAI; surgery if needed | RAI often preferred; surgery for large goitre | Symptomatic only (β-blockers, NSAIDs/steroids if painful) |
| ⚠️ Key Exam Pearls | Only cause with eye disease 👁️; smokers at higher risk | Commonest cause in elderly; no eye signs | Tender thyroid + ↓ uptake = classic! 📉 |
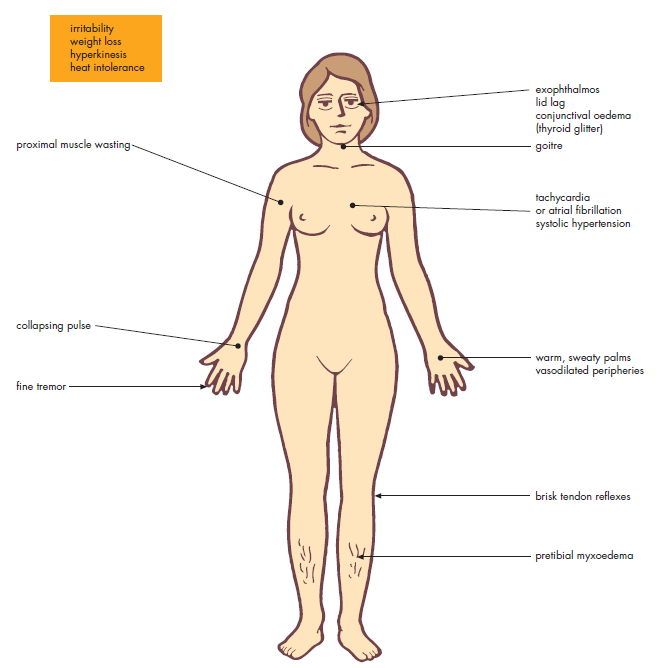
🩺 Clinical Features
- Weight loss ⚖️ despite ↑ appetite.
- Heat intolerance ☀️, sweating.
- Palpitations ❤️ (AF, tachycardia common).
- Neuro: anxiety, tremor, irritability.
- GI: diarrhoea, ↑ bowel frequency.
- Muscle: proximal myopathy 💪.
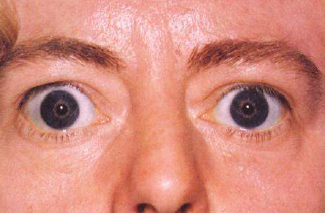
- Graves’ specific: Ophthalmopathy 👁️, pretibial myxoedema, thyroid acropachy.
🔬 Investigations
- ↑ Free T3/T4, ↓ TSH (except pituitary adenoma).
- TRAb positive → Graves.
- Other antibodies: anti-TPO, anti-TG (autoimmune thyroiditis).
- RAI uptake scan: diffuse (Graves) vs patchy (multinodular) vs focal (adenoma) vs ↓ uptake (thyroiditis).
- ECG: AF common → ↑ stroke risk 🧠.
- Other: mild ↑ Ca, ↑ ALP, ↓ K⁺ (periodic paralysis, esp. SE Asians).
💊 Management
- Symptomatic: – Propranolol 20–40 mg TDS (also ↓ T4→T3 conversion). – Useful for tremor, palpitations, anxiety.
- Antithyroid drugs 💊 – Carbimazole (1st line UK): start 20–40 mg OD → titrate to euthyroid (usual maintenance 5–15 mg). – Propylthiouracil (PTU): preferred in 1st trimester pregnancy; also blocks T4→T3 conversion. – Regimens: titration vs “block & replace” (carbimazole + thyroxine). – Duration: ~12–18 months, then trial withdrawal. ⚠️ Major adverse effect: agranulocytosis (0.5%) → fever/sore throat = urgent FBC + stop drug.
- Radioactive Iodine (I-131) ☢️ – Single dose effective in most. – Contraindicated in pregnancy & breastfeeding. – May worsen eye disease → avoid in active Graves’ orbitopathy (esp. smokers). – Hypothyroidism common post-treatment → lifelong thyroxine.
- Surgery 🔪 – Indications: large obstructive goitre, suspicious nodules, relapse after drugs/RAI, or pregnancy contraindicating RAI. – Risks: recurrent laryngeal nerve injury, hypocalcaemia (parathyroid removal).
🤰 Hyperthyroidism in Pregnancy
- Specialist endocrine + obstetric care required 👩⚕️.
- 1st trimester: PTU (less teratogenic).
- 2nd–3rd trimester: Carbimazole (preferred to avoid PTU hepatotoxicity).
- Surgery: 2nd trimester safest if needed.
- Uncontrolled thyrotoxicosis ↑ risk: miscarriage, pre-eclampsia, IUGR, stillbirth.
🚨 Thyroid Storm (Medical Emergency)
- Severe thyrotoxicosis with fever 🌡️, tachyarrhythmias ❤️, delirium 🧠, multi-organ failure.
- Precipitated by infection, surgery, trauma.
- Rx: – IV propranolol/esmolol (rate control). – PTU high dose (600–1000 mg load, then 200–300 mg q6h). – Lugol’s iodine after PTU (blocks release). – IV hydrocortisone (stress dose). – Supportive (fluids, cooling, ICU).
📚 References
- NICE CKS: Hyperthyroidism
- De Leo, Lee & Braverman. Hyperthyroidism. N Engl J Med 2016.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
