| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Clostridium tetani - Tetanus
Related Subjects:
|Pasteurella Multocida
|Capnocytophaga canimorsus
|Snake Bites
|Dog Bites
|Tetanus
When tetanus spores enter a suitable low-oxygen environment (soil-contaminated wounds, devitalised tissue), Clostridium tetani germinates and releases tetanospasmin - a lethal neurotoxin causing spastic paralysis. 🦠 Recovery does not confer immunity, so vaccination is always required after infection.
| 🚨 Initial Tetanus Management Summary |
|---|
|
📖 About
- Clostridium tetani is a Gram-positive, spore-forming anaerobe found in soil, dust, and animal waste.
- Disease results from tetanospasmin toxin → blocks inhibitory neurotransmitters (GABA, glycine) → sustained muscle contraction.
- Fatality rate: 20–60% (highest in neonates and elderly, often due to respiratory failure or autonomic instability).
- High-risk in areas with poor wound hygiene or inadequate immunisation programmes.
- No natural immunity: Even survivors must complete full tetanus toxoid vaccination. 💉
🔬 Microscopy
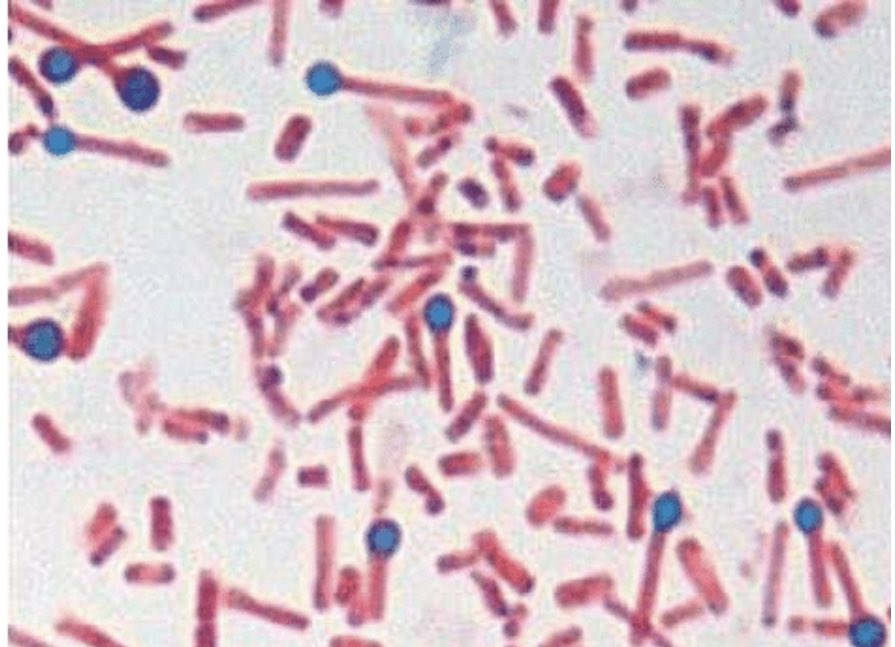
🧫 Characteristics
- Gram-positive, motile, obligate anaerobe.
- Spore-forming bacillus with a "drumstick" appearance (terminal spores).
- Produces:
- Tetanospasmin – neurotoxin (clinical tetanus).
- Tetanylisin – haemolysin, minor role in disease.
⚙️ Aetiology & Pathophysiology
- Transmission: Spores enter via puncture wounds, deep lacerations, burns, animal bites, or contaminated surgical wounds. Neonatal tetanus: via infected umbilical stump.
- Toxin action: Retrograde axonal transport → spinal cord → blocks inhibitory neurotransmitters (GABA, glycine) → unchecked motor neuron activity → spasms/rigidity.
- Incubation: 3–21 days (shorter = worse prognosis).
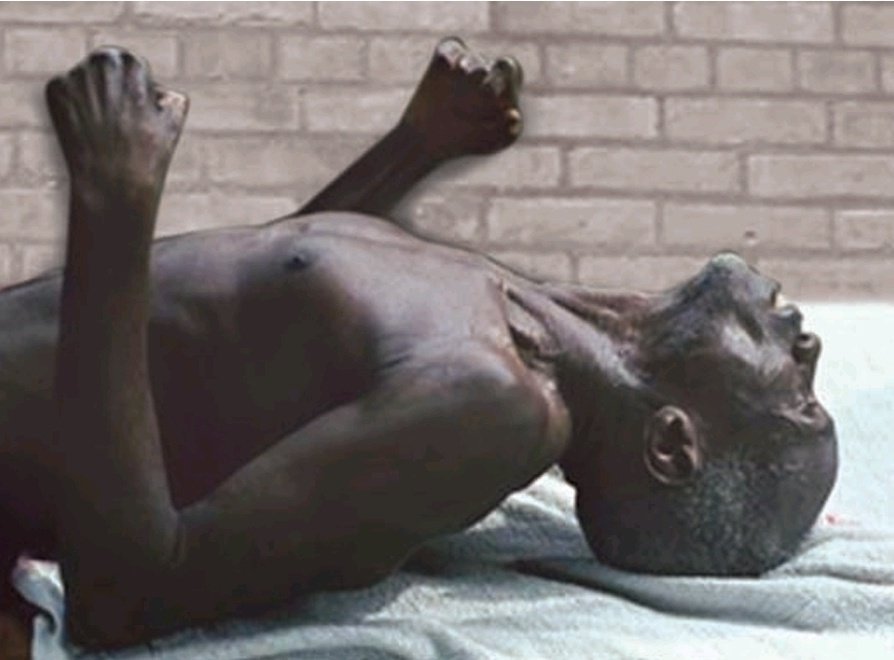
🩺 Clinical Presentation
- Trismus (lockjaw) 😬 – often first sign.
- Risus sardonicus – characteristic “sardonic smile.”
- Opisthotonus – severe arching of the back from spasm.
- Generalised rigidity, painful spasms triggered by minor stimuli (light, touch, noise).
- Autonomic features: tachycardia, labile hypertension, sweating, salivation, fever.
- Respiratory muscle involvement → hypoxia, arrest.
- Forms: Generalised, localised, cephalic, neonatal.
📊 Grading of Severity
- I (Mild): Trismus + rigidity, no spasms or respiratory compromise.
- II (Moderate): Rigidity + spasms, mild respiratory distress.
- III–IV (Severe): Frequent prolonged spasms, airway compromise, autonomic dysfunction.
🧾 Differential Diagnosis
- Strychnine poisoning: Glycine antagonist; mimics tetanus.
- Acute dystonia: Can cause trismus; resolves with anticholinergics (benztropine).
🔎 Investigations
- Primarily clinical diagnosis – lab confirmation is rare.
- Blood agar culture: poor, indistinct growth.
- Toxin assays confirm but not widely available.
- Check wound cultures – but often negative.
💉 Prevention
- Vaccination: Tetanus toxoid (part of UK DTaP schedule: 2, 3, 4 months + boosters at 3 yrs, 14 yrs).
- Wound prophylaxis: TIG for contaminated wounds if vaccination incomplete/uncertain.
- Neonatal tetanus: Prevented via maternal immunisation + clean delivery practices.
💊 Management
- Supportive Care: ABC support, ITU, tracheostomy/ventilation if needed.
- Sedation/Spasm control: Diazepam or midazolam IV; may require neuromuscular blockade + ventilation.
- Antitoxin: Human TIG 150 U/kg IM across multiple sites. (Equine TIG possible where human unavailable, but risk of anaphylaxis.)
- Antibiotics: IV metronidazole preferred. (Older studies showed penicillin may worsen spasms.)
- Wound Care: Debridement after TIG to remove necrotic tissue/spores.
- VTE prophylaxis in immobilised patients.
- Autonomic dysfunction: Morphine (sympathetic overdrive), labetalol (hypertension), inotropes (hypotension).
⚠️ Complications
- Respiratory failure from spasm.
- Autonomic dysregulation → labile BP, arrhythmias.
- Secondary infections (VAP, sepsis) in ITU.
- Fractures/dislocations from violent spasms.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
