| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Spinal Cord Infarction
Related Subjects: |Neurological History taking |Motor Neuron Disease (MND-ALS) |Miller-Fisher syndrome |Guillain Barre Syndrome |Multifocal Motor Neuropathy with Conduction block |Inclusion Body Myositis |Multiple Sclerosis (MS) Demyelination |Transverse myelitis |Acute Disseminated Encephalomyelitis |Cervical spondylosis |Spinal Cord Anatomy |Acute Disc Prolapse |Spinal Cord Compression |Spinal Cord Haematoma |Foix-Alajouanine syndrome |Cauda Equina |Conus Medullaris syndrome |Anterior Spinal Cord syndrome |Central Spinal Cord syndrome |Brown-Sequard Spinal Cord syndrome |Vitamin B12 deficiency |Myelopathy |Spinal Cord Arteriovenous Malformations
📖 About
- 🧠 Spinal cord infarction is a rare but severe cause of acute myelopathy, most often linked to aortic disease or surgery.
- ⚡ Classically presents as Anterior Spinal Artery Syndrome.
🩸 Vascular Supply
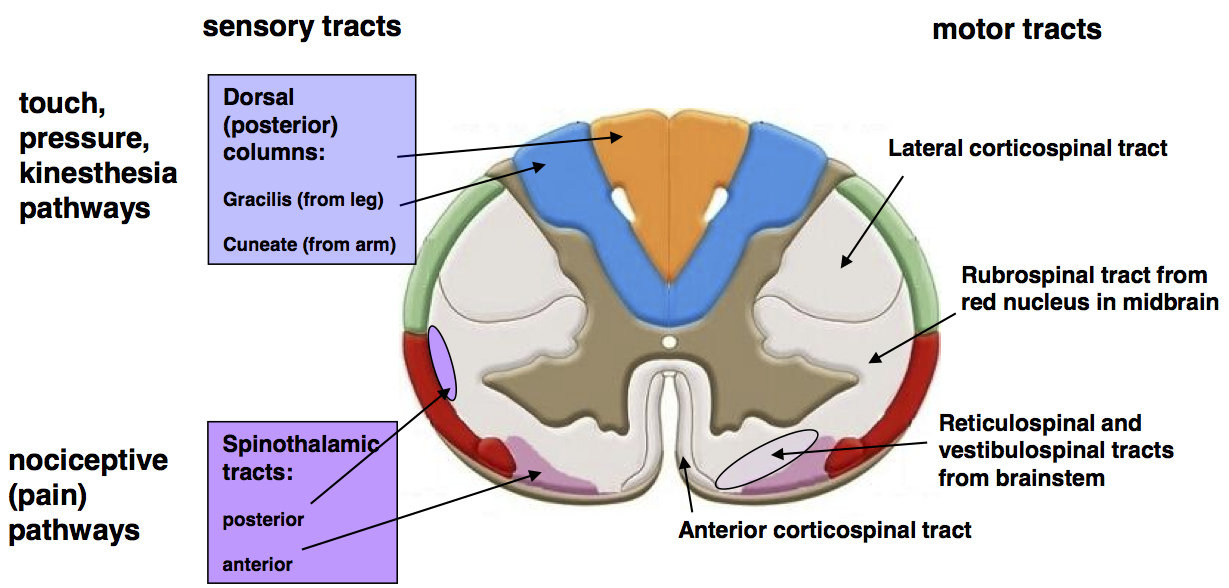
- Anterior Spinal Artery: Single vessel supplying anterior 2/3 of cord (motor tracts + spinothalamic pathways).
- Posterior Spinal Arteries: Paired vessels supplying posterior 1/3 (dorsal columns).
- Segmental Arteries: Aortic branches reinforce supply - most important is the Artery of Adamkiewicz (T6–L4), critical for lower cord perfusion.
- 🟡 The mid-thoracic cord is especially vulnerable → “watershed” zone with poor collateral supply.
🧩 Anatomy
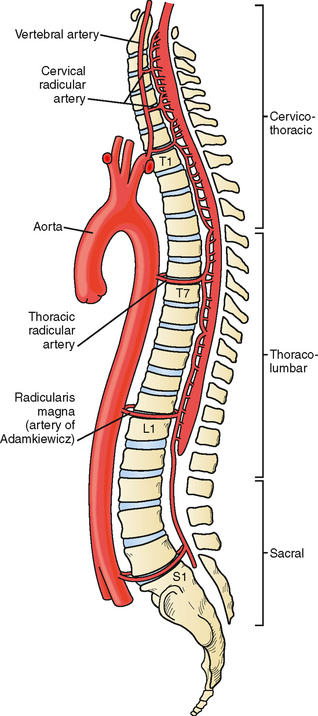
🧩 Cross Section
⚠️ Aetiology
- 🩻 Thoraco-abdominal aortic dissection.
- 🔪 Aortic aneurysm repair or cross-clamping.
- 🧪 Atherosclerotic vessel occlusion.
- 💔 Embolic events (e.g., atrial fibrillation, atheroembolism).
- Rare: systemic hypotension, vasculitis, coagulopathy.
🔬 Pathophysiology
- 🟥 Infarction typically affects anterior 2/3 of cord (corticospinal + spinothalamic tracts + anterior horn cells).
- 🟦 Posterior columns are spared → vibration & proprioception intact.
- “Disconnection syndrome”: profound motor and pain/temperature loss but preserved dorsal column sensation.
🩺 Clinical Presentation
- ♿ Sudden onset flaccid paraplegia → later spasticity.
- 🚽 Loss of bladder and bowel control.
- 🔥 Loss of pain and temperature sensation below lesion.
- 🎯 Preservation of vibration and proprioception (posterior column sparing).
- Onset often abrupt during/after aortic surgery or severe hypotension.
🚨 Red Flag: Sudden paraplegia following aortic surgery or dissection = spinal cord infarction until proven otherwise. Requires urgent MRI and vascular input.
🧪 Investigations
- 🖥 MRI spine (incl. diffusion-weighted) = most sensitive; may show “pencil-like” T2 hyperintensity.
- CT spine if MRI unavailable.
- 🩸 Bloods: screen for vascular risk (lipids, glucose, clotting, vasculitis screen if indicated).
- 🩻 CT or MR angiography → assess aortic and segmental vessel supply.
💊 Management
- Supportive Care: ABCs, oxygen, cardiovascular stabilisation.
- Pressure Care: Prevent sores with regular repositioning.
- Bowel/Bladder Management: Catheterisation, bowel regimen.
- VTE Prophylaxis: LMWH, stockings.
- Rehabilitation: Early physio, OT, mobility aids to maximise independence.
- Prevention: Careful aortic surgery technique, maintain cord perfusion pressure, avoid hypotension.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
