| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Granulomatosis with Polyangiitis GPA (Wegeners)✅
Related Subjects: Granulomatosis with Polyangiitis (GPA, formerly Wegener's) | Goodpasture's Syndrome (Anti-GBM Disease) | Respiratory Failure | Acute Kidney Injury
Early recognition and prompt immunosuppression are critical to prevent irreversible organ damage. If GPA is suspected, urgently request c-ANCA (PR3). Without treatment, GPA can destroy kidneys within weeks.
ℹ️ Overview
- 🧑⚕️ First described by Dr. Friedrich Wegener in 1936 (now renamed GPA due to historical associations).
- 📛 Granulomatosis with Polyangiitis (GPA) is a systemic necrotizing vasculitis affecting ENT, lungs, and kidneys.
- ⏱️ Untreated mortality: ~90% within 2 years.
🧬 Pathophysiology
- 🌡️ Autoimmune, small-to-medium vessel vasculitis, likely triggered by environmental antigens.
- 🦠 Staphylococcus aureus carriage increases relapse risk; eradication reduces recurrence.
- 🩺 Renal involvement: 40% at presentation, up to 90% over disease course.
- 🪢 Granulomatous inflammation → necrosis of affected tissues (ENT, lungs, kidneys).
📊 Epidemiology
- 👥 Incidence ~3/100,000 (USA); similar UK estimates.
- ⏱️ Mean age of onset ~50 yrs.
- ⚖️ M:F ratio = 1:1.
- 🌍 Predominantly Caucasian populations (~90%).
🧱 Granuloma Formation
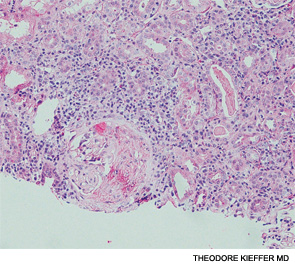
🩺 Clinical Features
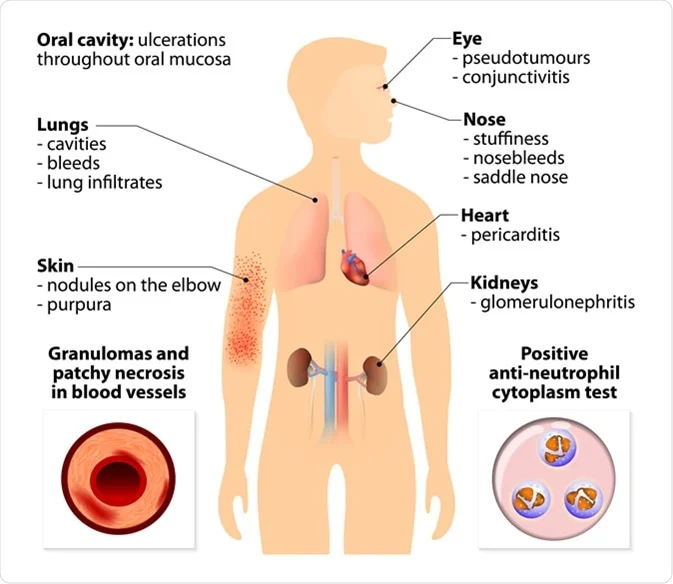
- 🛏️ Constitutional: fever, night sweats, malaise, fatigue.
- 👃 ENT: chronic sinusitis, epistaxis, otitis media, nasal septal perforation, saddle nose deformity.
- 🫁 Lungs: cough, haemoptysis, pulmonary haemorrhage (↑DLCO), nodules ± cavitation.
- 🧽 Kidneys: hypertension, haematuria, pauci-immune necrotizing glomerulonephritis.
- 👁️ Ocular: uveitis, scleritis, proptosis.
🔬 Investigations
- 🩸 FBC: anaemia, leukocytosis.
- 🧪 U&E: rising creatinine/urea; renal impairment.
- 🔥 ESR/CRP: elevated.
- 🧪 Complement: sometimes low.
- 🫁 CXR: nodules, infiltrates, cavitations, pulmonary haemorrhage.
- 🧫 Urinalysis: proteinuria, haematuria, dysmorphic RBCs, RBC casts.
- 🖥️ HRCT chest: alveolar haemorrhage, nodules, airway stenosis.
- 🔑 ANCA serology: c-ANCA (PR3) positive 80–90% (correlates with activity), p-ANCA (MPO) positive 10–20%.
- 🔍 Biopsy (ENT/lung/kidney): necrotizing granulomatous vasculitis.
- 🫁 BAL: blood in alveoli for pulmonary haemorrhage.
- 💨 DLCO: increased in alveolar haemorrhage due to Hb CO-binding.
🖼️ Imaging
📸 CT: multiple cavitary (arrows) and non-cavitary (arrowheads) pulmonary nodules typical of GPA.
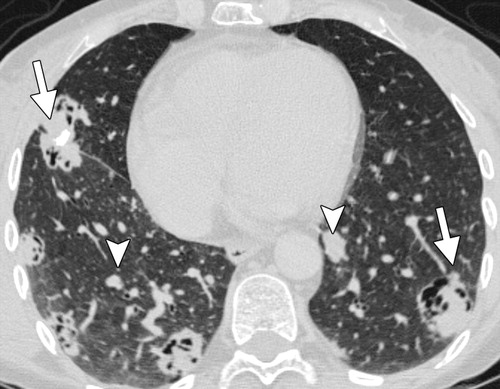
💊 Management
- ⚠️ Untreated mortality ~90% at 2 years; early treatment dramatically improves survival.
- Induction therapy: • Severe/organ-threatening: high-dose corticosteroids + cyclophosphamide (CYC) or rituximab (RTX). • Non-severe: methotrexate (MTX) or RTX ± steroids.
- Maintenance therapy: azathioprine, MTX, or RTX (especially PR3+ high-risk relapsers). • RTX infusions can extend up to 42 months for high relapse risk.
- Adjunctive therapy: • Co-trimoxazole prophylaxis (for Pneumocystis and reduces Staph. nasal colonisation). • Long-term mupirocin nasal therapy. • Plasma exchange (PLEX) if severe renal disease (Cr >500 μmol/L) or pulmonary haemorrhage.
Case – Granulomatosis with Polyangiitis (GPA)
42M with chronic sinusitis, epistaxis, conductive hearing loss, pleuritic chest pain, blood-streaked sputum, fatigue, and ankle oedema. Exam: saddle nose, crackles; BP 158/92. Labs: normocytic anaemia, rising creatinine, RBC casts; CXR: multiple cavitating nodules. Serology: strongly positive c-ANCA (PR3). Nasal/renal biopsy: necrotising granulomatous vasculitis. Management: IV methylprednisolone → high-dose oral taper + rituximab (or cyclophosphamide), PPI, bone protection, PJP prophylaxis. Consider plasmapheresis if severe pulmonary haemorrhage or dialysis-dependent RPGN. Maintenance with rituximab/azathioprine; multidisciplinary follow-up (ENT, respiratory, nephrology). Monitor for relapse and treatment toxicity. Differentials: microscopic polyangiitis, EGPA, infection (TB/fungal), malignancy.
📚 References
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
