| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Small Bowel Obstruction (Adults)
Related Subjects: Small Bowel Obstruction |Colonic (Large bowel) Obstruction |Caecal Volvulus |Small Bowel Ischemia |Hartmann's procedure |Sigmoid Volvulus |Acute Colonic Pseudo-obstruction |
🚨 Small Bowel Obstruction (SBO) is a surgical emergency. It most often arises from adhesions after previous laparotomy, but can also result from hernia, Crohn’s disease, or intussusception. ⚠️ Diagnosis is often delayed, leading to perforation, sepsis, and high mortality if not recognised early.
| 🩺 Initial Management of SBO |
|---|
|
📖 About
- SBO is one of the most common causes of acute surgical admission.
- Can present as total (complete) or subtotal (partial) obstruction.
- Mortality is driven by ischaemia and perforation → rapid recognition is vital.
🧬 Aetiology
- Pathophysiology: Obstruction → proximal bowel dilatation, bacterial overgrowth, fluid sequestration → perforation risk at maximum diameter site (usually caecum).
- Strangulation impairs blood supply → necrosis and sepsis.
🔎 Causes
- Luminal: Tumour, gallstone ileus, foreign body, bezoar, faecal impaction.
- Mural: Crohn’s stricture, neoplasm, radiation stricture, ischaemia, pseudo-obstruction.
- Extramural: Adhesions (most common in UK), hernias, volvulus, intussusception, peritoneal TB, pelvic/ovarian malignancy.
👩⚕️ Clinical Features
- Symptoms: Colicky central abdominal pain, bilious vomiting, abdominal distension, constipation/obstipation.
- Signs: Dehydration, tachycardia, tender/distended abdomen, high-pitched "tinkling" bowel sounds. Late → peritonitis, shock, sepsis.
🧪 Investigations
- Bloods: FBC, U&E, lactate, amylase, CRP. Raised lactate → ischaemia/strangulation.
- AXR: Dilated central loops, valvulae conniventes across lumen, fluid levels.
- CXR: Free air under diaphragm = perforation.
- CT abdomen: Transition point, closed loop obstruction, evidence of strangulation.
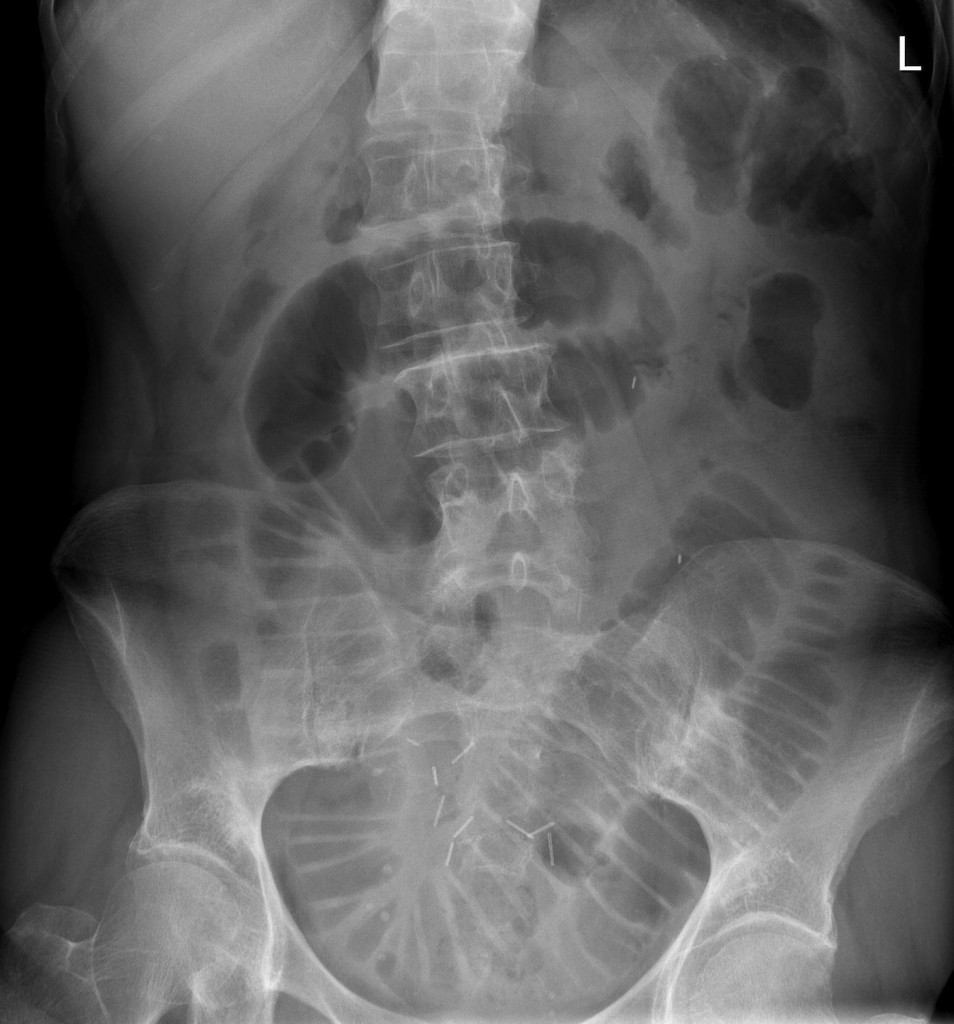
📷 Example AXR
The valvulae conniventes are clearly demonstrated. Central distended small bowel loops with visible old surgical staples. Cause: adhesions.
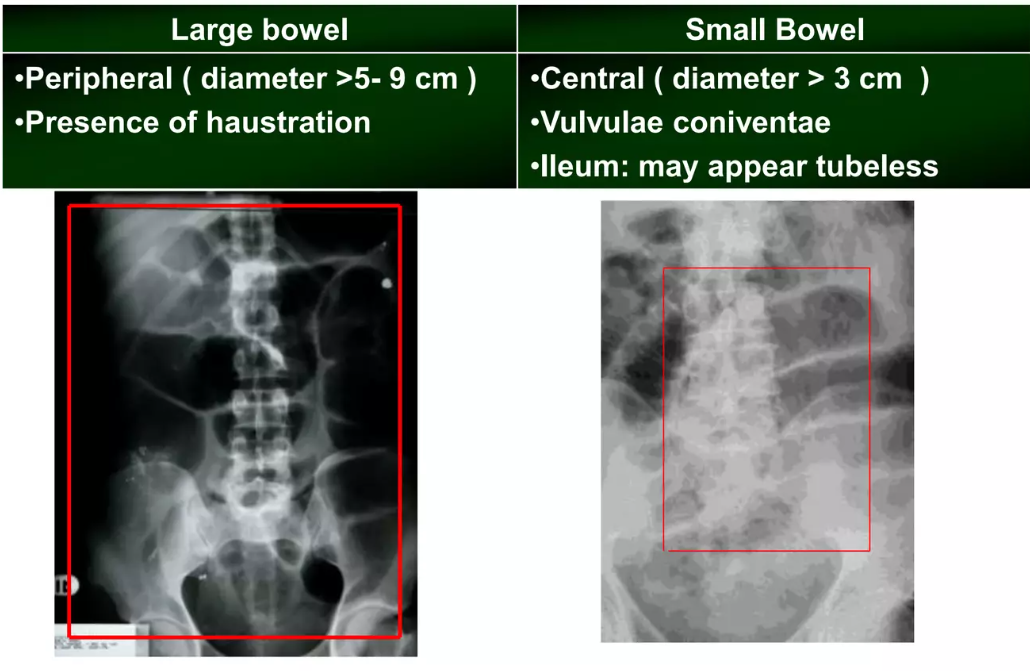
📊 Comparison: Small vs Large Bowel Obstruction
| Feature | Small Bowel | Large Bowel |
|---|---|---|
| Abdominal Pain | Early, colicky, central | Dull, less colicky |
| Vomiting | Early bilious, late faeculent | Occurs later |
| Constipation | Late feature | Early, may pass diarrhoea if partial |
| Distension | Less if high obstruction; marked if distal | Marked, esp. sigmoid/caecal volvulus |
| Bowel Sounds | High-pitched "tinkling" | Often reduced or absent late |
| AXR | Central dilated loops, valvulae conniventes across bowel | Peripheral dilatation, haustra not spanning full lumen |
| Common Causes | Adhesions, hernia, Crohn’s, volvulus | Colorectal cancer, sigmoid volvulus, diverticular disease |
💊 Management
- Resuscitation: IV fluids, electrolyte correction, catheterisation.
- Decompression: NG tube on free drainage.
- Antibiotics: Broad-spectrum (gram-negative + anaerobes) if perforation or sepsis suspected.
- Surgical intervention: Emergency laparotomy for peritonitis, perforation, or ischaemia. Adhesiolysis or resection depending on cause.
- Medical: Conservative trial if partial obstruction (esp. adhesions) with close monitoring.
- Palliative: For advanced malignancy or poor surgical candidates.
📚 References
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
