| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Acute Anaphylactoid Reactions
Related Subjects: Atropine |Acute Anaphylaxis |Basic Life Support |Advanced Life Support |Adrenaline (Epinephrine) |Acute Hypotension |Cardiogenic shock |Distributive Shock |Hypovolaemic or Haemorrhagic Shock |Obstructive Shock |Septic Shock and Sepsis |Shock (General Assessment) |Toxic Shock Syndrome
⚡ Emergency Reminder: In suspected anaphylaxis give Adrenaline (Epinephrine) immediately. Dose: 0.5–1 mg (0.5–1 mL of 1:1000) IM into the lateral thigh using a long needle to reach muscle. 💉 Adrenaline is life-saving – do not delay for IV access or investigations.
| 🚑 Initial Management Summary |
|---|
|
🔎 About
- These reactions resemble acute anaphylaxis but are non–IgE mediated.
- Unlike true allergy, risk does not increase with repeat exposure.
- Some drugs may be cautiously reintroduced if essential (e.g. acetylcysteine in paracetamol overdose).
🧬 Aetiology (Pathophysiology)
- No cross-linking of IgE antibodies on mast cells.
- Instead there is direct mast cell degranulation → histamine & mediator release.
- This explains why skin, gut, and cardiovascular features look identical to IgE reactions.
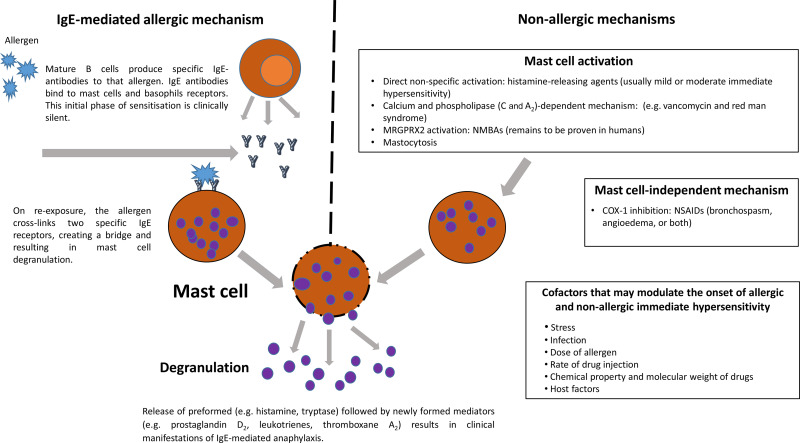
💊 Common Causative Agents
- Opiates (e.g. morphine)
- Aspirin & NSAIDs
- Acetylcysteine (Parvolex)
- Radiocontrast media (CT, angiography)
- Exercise, cold-induced reactions
🩺 Clinical
- Indistinguishable from IgE anaphylaxis: urticaria, hypotension, bronchospasm, GI upset.
- Key learning point: manage identically in the acute phase.
🔬 Investigations
- ⬆️ Raised mast cell tryptase (peaks at 1–2 hrs, supports diagnosis).
- ❌ Negative specific IgE tests (helps differentiate from true allergy).
🛠️ Management
- 💉 Same acute management as anaphylaxis – adrenaline is first line.
- ✅ Once stabilised, careful review: drug may be restarted under supervision if essential.
- 📋 Always document the event and advise patient about future precautions.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
