| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Thyroid Eye Disease
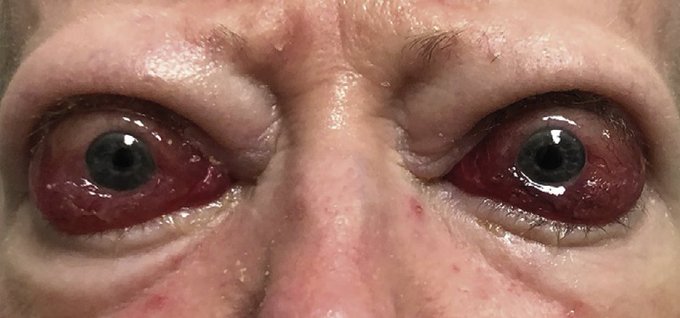
👁️ Thyroid Eye Disease (TED) (Graves’ orbitopathy) is an autoimmune inflammatory disorder of the orbit, most often associated with Graves’ disease. Orbital fibroblast activation (driven by thyroid autoimmunity) leads to glycosaminoglycan deposition and expansion of extra-ocular muscles and orbital fat → lid retraction ⬆️, proptosis 🤯, exposure symptoms 💧, and restrictive diplopia 👀. Management depends on activity (inflamed “active” vs stable “inactive”) and severity (mild vs moderate–severe vs sight-threatening).
🔬 Pathophysiology (why it happens)
- Autoimmune activation of orbital fibroblasts causes cytokine-mediated inflammation plus accumulation of glycosaminoglycans (water-binding “gel”) → oedema and tissue expansion.
- Extra-ocular muscle enlargement (classically belly > tendon) + fat expansion increases orbital volume/pressure → proptosis and motility restriction (diplopia).
- Sight-threatening TED is mainly due to:
- 🧠 Dysthyroid optic neuropathy (DON) from apical crowding/compression.
- 💧 Severe exposure keratopathy causing corneal ulceration/perforation risk.
Mentor point: think of severe TED as an orbital compartment problem—swollen tissues raise pressure and can threaten the optic nerve and cornea.
⚡ Risk factors
- 🚬 Smoking (strongest modifiable risk factor; increases severity and reduces treatment response).
- 🔄 Uncontrolled thyroid status (swings in thyroid function can worsen TED; aim for stable euthyroidism).
- ☢️ Radioiodine (RAI) can precipitate or worsen TED in some people.
🩺 Clinical presentation (mild → sight-threatening)
- Mild: gritty/dry eyes, watering, photophobia, conjunctival redness, lid retraction, periorbital swelling, mild proptosis.
- Moderate–severe: troublesome proptosis, persistent diplopia (restrictive myopathy), significant inflammation/chemosis, exposure keratopathy.
- Sight-threatening RED FLAGS 🚨 (same-day assessment):
- ⬇️ Reduced visual acuity or colour desaturation (early DON clue).
- 🟠 RAPD, new visual field defect, or optic disc swelling (DON can occur with a normal disc early).
- 💥 Corneal ulceration, inability to close the lids (lagophthalmos), severe ocular pain/photophobia.
🔎 Diagnosis (practical work-up)
- Eye assessment: visual acuity, colour vision, pupils/RAPD, ocular motility & diplopia, lid position, corneal staining, fundus exam; exophthalmometry if available.
- Thyroid tests: TFTs ± TRAb to support Graves’ aetiology.
- Imaging (moderate–severe/atypical/DON concern): CT/MRI orbits to assess muscle enlargement and apical crowding/optic nerve compression.
- Visual fields if DON suspected or to establish baseline in significant disease.
💊 Management (NICE-aligned principles + specialist TED pathways)
1) Start immediately (all severities)
- 🚭 Smoking cessation (biggest modifiable factor).
- 🎯 Restore and maintain euthyroidism (coordinate with endocrinology).
- 💧 Corneal protection: preservative-free lubricants by day + ointment at night; consider lid taping/moisture chamber if exposure.
- 🕶️ Sunglasses; head elevation at night; treat blepharitis/dry eye.
2) Hyperthyroidism treatment choice (key NICE point)
- Avoid radioactive iodine as first-line definitive therapy when active thyroid eye disease is present (choose alternatives such as antithyroid drugs or surgery as clinically appropriate).
- When discussing definitive therapy, include the risk of precipitating/worsening thyroid eye disease as part of shared decision-making.
3) Moderate–severe, active TED (specialist-led)
- IV glucocorticoids are generally preferred over oral regimens for active, moderate–severe disease.
- Other immunomodulatory options (often in specialist centres) may be used depending on response, phenotype, and contraindications.
- Consider orbital radiotherapy in selected cases (typically alongside medical therapy, specialist decision).
4) Sight-threatening TED (emergency)
- Suspected DON or severe corneal exposure/ulceration → urgent same-day ophthalmology.
- Specialist pathways commonly use high-dose IV methylprednisolone urgently; if inadequate response, urgent orbital decompression may be required.
🧩 Disease phases (how to explain it to learners)
- 🔥 Active/inflammatory phase: treat inflammation + protect the cornea + stabilise thyroid status + stop smoking.
- 😴 Inactive/quiescent phase: rehabilitative correction of residual problems (strabismus surgery, orbital decompression for appearance/proptosis, lid surgery) once stable.
🧠 Key clinical pearls
- DON is a clinical diagnosis—don’t wait for imaging if vision/colour vision is dropping.
- Corneal protection prevents avoidable morbidity while you arrange specialist care.
- RAI and TED: NICE highlights TED risk and advises RAI is unsuitable when TED is active; this is a common exam and real-world pitfall.
📚 Sources
- NICE NG145 Thyroid disease: assessment and management (includes TED considerations and notes RAI may be unsuitable in active thyroid eye disease).
- EUGOGO 2021 Clinical Practice Guidelines (severity/activity framework; emergency management of DON; IV methylprednisolone and escalation principles).
- Patient.info (Doctor) Thyroid eye disease overview (clinical features and practical UK-facing summary).
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
