| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Acute Cholecystitis ✅
Related Subjects:Acute Cholecystitis |Acute Appendicitis |Chronic Peritonitis |Abdominal Aortic Aneurysm |Ectopic Pregnancy |Acute Cholangitis |Acute Abdominal Pain |Penetrating Abdominal Trauma |Acute Pancreatitis |Acute Diverticulitis
⚠️ Mortality: Acute calculous cholecystitis has <10% mortality with prompt hospital management. However, 🔥 Acute Acalculous Cholecystitis (more common in critically ill/ICU patients) carries a mortality up to 50% 🚨 and requires urgent recognition and intervention. 💡 Teaching Tip: Always distinguish calculous from acalculous; high mortality in ICU means early suspicion is lifesaving.
| 🩺 Initial Management Summary |
|---|
|
ℹ️ About
- 📊 Prevalence: Gallstones affect ~10% of the population; 10–20% symptomatic.
- 🧪 Pathophysiology: Cystic duct obstruction → ↑ intraluminal pressure → bile stasis → gallbladder wall inflammation. 💡 Tip: Remember Charcot’s triad for cholangitis differs from Murphy’s sign for cholecystitis.
- 👩 Demographics: More common in women; incidence rises with age (♀ 24%, ♂ 15% by 70 years).
- 🔪 Treatment: Symptomatic patients usually require laparoscopic cholecystectomy after CBD stones excluded.
🧪 Aetiology
- 💧 Lithogenic bile: ↑ cholesterol, ↓ bile salts → stone formation.
- 🚪 Cystic duct obstruction: Primary trigger → gallbladder inflammation.
- 🦠 Secondary infection: Often E. coli, Klebsiella, Enterococcus.
- ⚠️ Empyema: Pus-filled gallbladder → urgent surgery. 💡 Exam Tip: Empyema = sepsis risk; do not delay surgery for antibiotics alone.
⚠️ Risk Factors
- 👵 Age >50, 👩 Female, Caucasian
- 🍔 Obesity, rapid weight loss, diabetes, metabolic syndrome
- 🧬 Crohn’s (terminal ileum), cholestyramine therapy
- 🤰 Pregnancy, cystic fibrosis
💎 Types of Gallstones
| Type | Description | Incidence |
|---|---|---|
| ⚪ Mixed | Cholesterol + bile salts + calcium; most common. | 70% |
| 🟡 Cholesterol | Solitary; linked with hyperlipidaemia, pregnancy; “strawberry GB”. | 20% |
| ⚫ Pigment | Dark; associated with haemolysis (e.g., sickle cell). | 5% |
| 🟤 Brown | Linked to infection (Clonorchis); rare in UK. | Rare |
Cholecystitis Imaging (USS & CT)
Oblique coronal US: thickened GB wall, pericholecystic fluid, impacted calculus in GB neck. LI = liver.
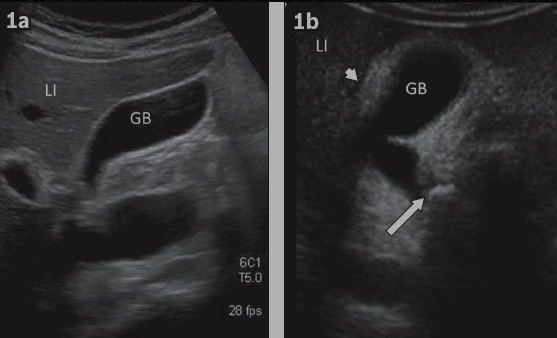
CT axial/coronal: thickened GB wall, pericholecystic fat stranding (white arrow), reactive hyperaemia in adjacent liver (black arrow); large calculus visible.
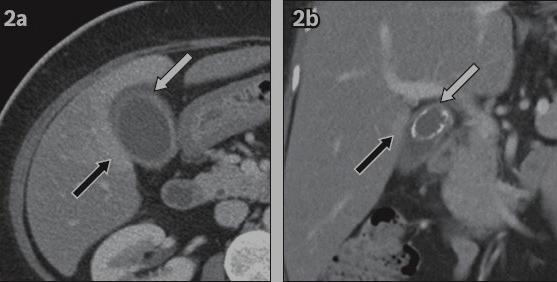
🩺 Clinical Features
- ⚡ Sudden, severe RUQ pain → radiates to right shoulder/scapula
- 🤮 Nausea, vomiting, anorexia, fever
- 🖐️ Murphy’s sign: Inspiratory arrest on RUQ palpation
- 🟡 Jaundice → consider CBD stone/cholangitis 💡 Teaching Tip: Pain + Murphy’s sign is classic; jaundice suggests a different pathology or complication.
🔎 Investigations
- 🧪 Bloods: leukocytosis, ↑ CRP, mildly deranged LFTs; ↑ bilirubin if CBD involved
- 🖥️ USS: 1st-line → stones, wall thickening, pericholecystic fluid, sonographic Murphy’s sign
- 🩻 CT: complications (abscess, perforation)
- 💿 MRCP: best for CBD stones
- 🛠️ ERCP: diagnostic + therapeutic for CBD stones
📐 Calot’s Triangle: Cystic duct, common hepatic duct, cystic artery. Identify clearly to avoid bile duct injury during surgery. 💡 Exam Tip: Knowledge of anatomy reduces iatrogenic injury risk.
🚨 Complications
| Complication | Presentation | Management |
|---|---|---|
| 🧴 Gallbladder empyema | Persistent RUQ pain, high fever/rigors, sepsis | Sepsis 6 → IV fluids, blood cultures, antibiotics + urgent cholecystectomy/percutaneous cholecystostomy if high risk |
| 🦴 Gangrenous cholecystitis | Severe RUQ pain, systemic toxicity | Resuscitate, IV antibiotics, urgent cholecystectomy (senior input) |
| 💥 Emphysematous cholecystitis | Severe pain, sudden sepsis, often diabetics | Immediate resuscitation, IV antibiotics, urgent surgery/cholecystostomy |
| 🕳️ Perforation | Worsening pain, peritonism, sepsis | Sepsis management + urgent surgery; consider percutaneous drainage if localised |
| 🧫 Pericholecystic collection/abscess | Persistent RUQ pain/fever, palpable mass | IV antibiotics, image-guided drainage ± delayed cholecystectomy |
| 🟡 Choledocholithiasis | Jaundice, pale stools, dark urine, intermittent RUQ pain | Risk stratify (LFTs/USS/MRCP), ERCP extraction, cholecystectomy |
| 🚑 Ascending cholangitis | Charcot triad: fever, RUQ pain, jaundice; ± hypotension/confusion (Reynolds pentad) | Sepsis 6 + IV antibiotics, urgent biliary decompression (ERCP/PTC) |
| 🫀 Gallstone pancreatitis | Epigastric pain radiating to back, vomiting, ± jaundice | Supportive care, ERCP if cholangitis/obstruction, cholecystectomy during index admission if feasible |
| 🔒 Mirizzi syndrome | Obstructive jaundice ± RUQ pain | Specialist imaging, HPB input, definitive surgery |
| 🔁 Cholecystoenteric fistula / gallstone ileus | Older patient, SBO, vomiting/distension | Resuscitation, NG tube, urgent surgery: enterolithotomy ± staged fistula repair |
| 🎯 Gallbladder carcinoma | Persistent RUQ pain, weight loss, anorexia, jaundice | Urgent referral, CT staging, HPB MDT management |
🎭 Differentials
- Peptic ulcer disease, liver abscess
- Acute pancreatitis
- MI (atypical pain), pneumonia (referred pain)
💊 Management
- 💉 Analgesia (IV morphine/alternative), NBM
- 🧪 IV antibiotics (cefuroxime + metronidazole / local protocol)
- 🔪 Laparoscopic cholecystectomy = definitive treatment (ideally 24–72 h)
- ⏳ Delayed surgery (~6 weeks) if high-risk/unstable
- 🛠️ ERCP for CBD stones prior to surgery 💡 Teaching Tip: Definitive surgery is key; antibiotics alone are not curative.
👵 Frail / Elderly Patients
⚠️ Atypical Presentation: In frail or elderly patients, acute cholecystitis often presents without classic signs. Fever and Murphy’s sign may be absent, and confusion, lethargy, or reduced oral intake may be the main features. 💡 Teaching Tip: Always consider acute cholecystitis in frail patients with unexplained delirium or functional decline. 🩺 Management Considerations: Careful ABC assessment, IV fluids, analgesia, and IV antibiotics remain first-line.💡 Surgical decisions require MDT input (geriatrician + surgeon) considering comorbidities and physiological reserve and patient choice. Failure to settle conservatively then INR to place a percutaneous cholecystostomy is often preferred if operative risk is high, with delayed elective cholecystectomy once stabilized. Some very frail patients may not be fit for either.
📚 References
Case – Acute Cholecystitis
46-year-old woman presents with RUQ pain radiating to back, fever, nausea after fatty meal. Positive Murphy’s sign, raised WBC/CRP, mildly cholestatic LFTs. USS: gallstones, wall thickening, pericholecystic fluid. Managed with ABCDE, IV fluids, analgesia, NBM, IV antibiotics (co-amoxiclav or cefuroxime + metronidazole if penicillin allergy), and early laparoscopic cholecystectomy (24–72 h). Consider percutaneous cholecystostomy if unstable. Monitor for complications: empyema, gangrene/perforation, CBD stones. Differentials: biliary colic, ascending cholangitis, gallstone pancreatitis. 💡 Exam Tip: Always link clinical features, labs, imaging, and management when answering short-answer or OSCE questions.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
