| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Platelets
Related Subjects: |Iron deficiency Anaemia |Haemolytic anaemia |Macrocytic anaemia |Megaloblastic anaemia |Microcytic anaemia |Myelodysplasia |Myelofibrosis |Hereditary Spherocytosis |Hereditary Elliptocytosis |Haemophilia A |Haemophilia B |Haemolytic anaemia |Heme |Globins |Red blood cells |White blood cells |Lymphocytes |Platelets |Cryoprecipitate |Fresh Frozen Plasma |Blood Cell Maturation |Blood film interpretation |Reticulocytes
🩸 About Platelets
- Platelets (thrombocytes) are small, disc-shaped cell fragments essential for clotting and wound healing.
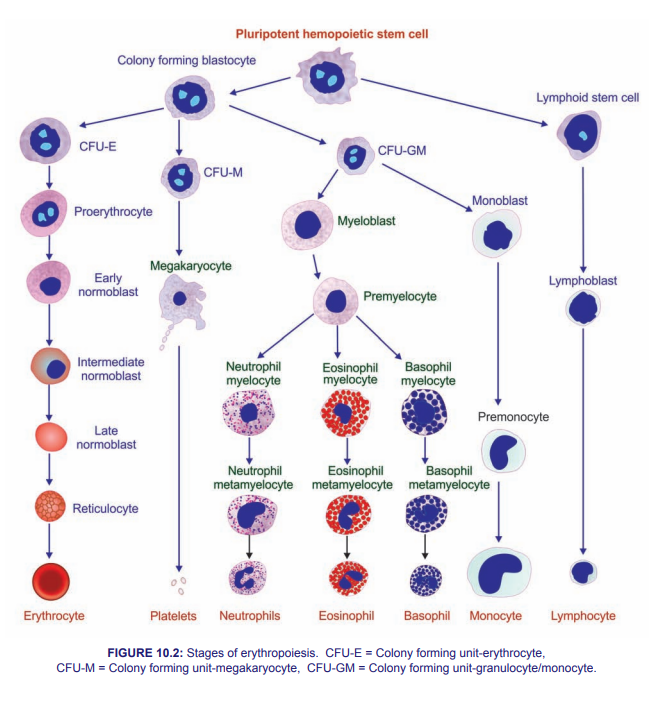
- Produced in the bone marrow from megakaryocytes.
- Circulate for 7–10 days before being cleared by spleen/liver.
- Main role: maintain hemostasis by forming platelet plugs at vessel injury sites.
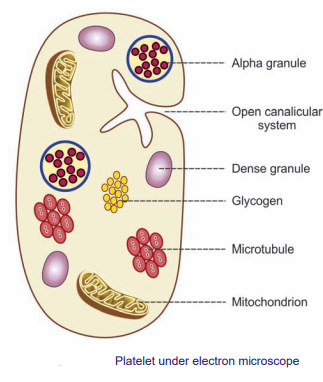
🔬 Structure of Platelets
- Size: 2–3 μm, anucleate but highly specialized.
- Peripheral Zone: Phospholipid membrane with glycoprotein receptors (GPIb, GPIIb/IIIa) → bind vWF & fibrinogen for adhesion/aggregation.
- Sol-Gel Zone: Actin + myosin cytoskeleton → shape change from smooth discs → spiky activated platelets.
- Organelle Zone: Alpha granules (growth factors, fibrinogen), Dense granules (ADP, serotonin, Ca²⁺), Lysosomes (enzymes).
⚙️ Function in Hemostasis
- Adhesion: Bind to exposed collagen via vWF + GPIb receptors.
- Activation: Shape change + granule release (ADP, thromboxane A₂) → recruits more platelets.
- Aggregation: GPIIb/IIIa binds fibrinogen → platelets cross-linked → temporary plug formed.
- Also release growth factors (PDGF, TGF-β) aiding tissue repair.
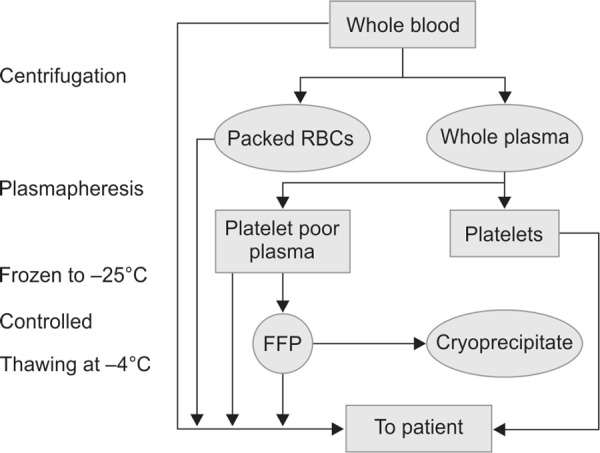
💉 Platelet Transfusion
- Pooled Platelets: From 4–6 whole blood donations; ~240,000 platelets/unit.
- Single Donor (Apheresis): From one donor; ~550,000 platelets/unit → ↓ risk of alloimmunisation.
- Storage: 20–24 °C, constant agitation; must be transfused within 4 hours of issue.
- Platelets ideally ABO- and Rh-compatible, but group-compatible units may be used if necessary.
🚨 Indications
- Active bleeding: if platelets <50,000/mm³; <100,000/mm³ for CNS/eye surgery.
- Prophylaxis in thrombocytopenia:
- <10,000/mm³ (no risk factors).
- <20,000/mm³ (with risk factors e.g. fever, infection).
- Massive transfusion protocols or post-cardiopulmonary bypass.
📊 Clinical Guidelines
- Transfuse ~4 pooled units (≈250 mL each) over 30–60 min.
- Check platelet count 1 hour post-transfusion to assess increment.
- Use Rh-negative platelets in Rh-negative patients (especially females of childbearing potential).
✅ Conclusion
- Platelets are central to clotting & healing 🩹.
- Platelet transfusion is life-saving in bleeding, thrombocytopenia, and peri-operative care.
- Best practice: correct indication, correct storage, and compatibility matching for safety.
📚 References

Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
