| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Arrhythmogenic Right Ventricular Cardiomyopathy
Related Subjects: |Ventricular Tachycardia |Right Ventricular Outflow Tract Tachycardia |Resuscitation - Adult Tachycardia Algorithm |Automatic Implantable Cardioverter Defibrillator (AICD)
⚡ ARVC is part of the group of arrhythmogenic cardiomyopathies, characterised by fibrofatty replacement of the myocardium, most commonly the right ventricle. It carries a major risk of sudden cardiac death (SCD) due to malignant ventricular arrhythmias, particularly during exertion. 📌 Early recognition and consideration of ICD implantation is essential.
📖 About
- Also known as Arrhythmogenic Right Ventricular Dysplasia (ARVD).
- Initially affects the right ventricle, but studies show progressive left ventricular involvement over time → can become a biventricular disease.
- Prevalence: ~1 in 5,000–10,000 (likely underdiagnosed).
- Important cause of sudden cardiac arrest in young athletes. 🏃♂️⚠️
🧬 Genetics
- Usually autosomal dominant inheritance with variable penetrance.
- More than 8 implicated genes, mostly affecting desmosomal proteins (responsible for cell–cell adhesion in myocardium).
- Ask about family history of arrhythmia or sudden unexplained death.
- Accounts for up to 20% of sudden cardiac deaths in young people.
🧪 Key Genes
- Plakophilin-2 (PKP2)
- Desmoplakin (DSP)
- Desmoglein-2 (DSG2)
- Desmocollin-2 (DSC2)
- Plakoglobin (JUP)
- TMEM43
- RYR2 (linked to calcium handling abnormalities)
📸 ECG – Epsilon Waves
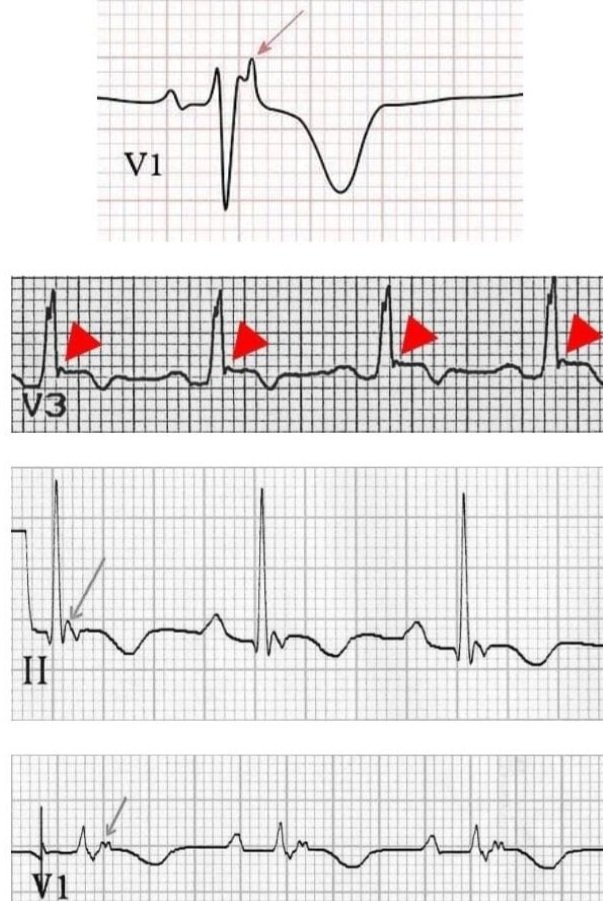
🩺 Aetiology / Pathology
- Mutations in desmosomal proteins weaken mechanical junctions → myocyte detachment & death → fibro-fatty replacement of myocardium.
- Predominantly affects RV free wall, outflow tract, and apex (“triangle of dysplasia”).
- Progressive thinning of RV wall → aneurysm formation → arrhythmia substrate.
- Subtypes: RV-dominant, biventricular, and LV-dominant ARVC.
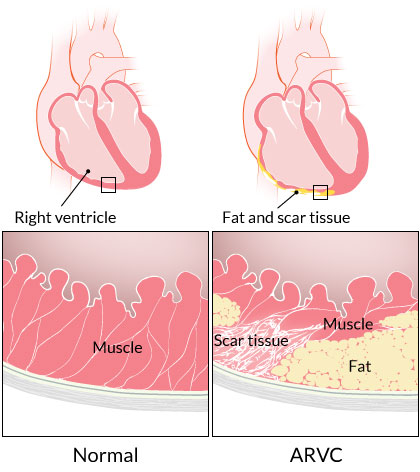
🩺 Clinical Features
- Palpitations/fluttering (ectopics, atrial fibrillation, ventricular tachycardia).
- Exertional syncope or chest pain.
- Dyspnoea from RV failure in advanced disease.
- Dizziness, fatigue, abdominal discomfort from hepatomegaly / venous congestion.
- Exam: Widely split S2, S3 or S4 gallop; later signs of right heart failure.
⚠️ Complications
- Arrhythmias → ventricular ectopics, AF, VT, VF (leading cause of death).
- Progressive biventricular heart failure.
- Bradyarrhythmias, AV block.
- Sudden cardiac death, often during exertion.
🔍 Investigations
- ECG: T-wave inversion in V1–V3, epsilon waves (terminal notching), incomplete RBBB, VT with LBBB morphology.
- Echocardiogram: RV dilation, akinesis/dyskinesis, prominent trabeculations, RVOT dilatation.
- Cardiac MRI: gold standard → RV structural/functional abnormalities + tissue characterization (fibrofatty infiltration).
- Holter/monitoring: detect ventricular arrhythmias of RV or LV origin.
- Endomyocardial biopsy: rarely used, limited sensitivity due to patchy disease.
🔎 Differentials
- Idiopathic RV outflow tract tachycardia (benign, no fibrosis).
- Brugada syndrome (channelopathy with similar arrhythmia risk).
- RV volume overload from congenital lesions (e.g., ASD, Ebstein anomaly).
📸 ECG Showing Epsilon Waves
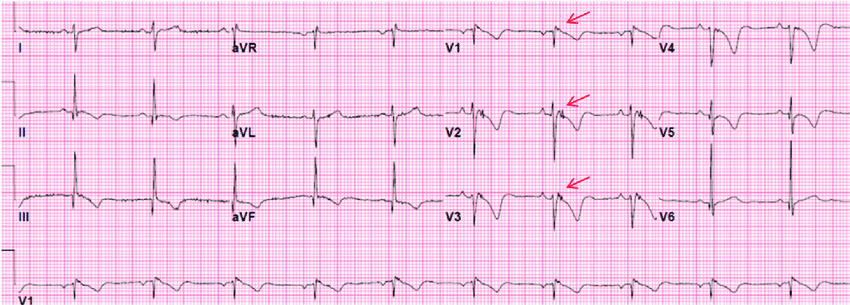
👨👩👧 Screening
- All first-degree relatives: 12-lead ECG + cardiac imaging; consider signal-averaged ECG.
- Genetic testing if pathogenic variant identified in proband.
- Family follow-up essential as penetrance increases with age.
💊 Management
- Lifestyle: Avoid competitive or high-intensity sports, caffeine, stimulants. Moderate daily activity only.
- ICD: definitive therapy for high-risk or survivors of cardiac arrest / sustained VT.
- Antiarrhythmics: beta-blockers (mainstay), sotalol, amiodarone for VT suppression.
- Catheter ablation: option for recurrent VT refractory to drugs; often palliative (high recurrence).
- Heart failure therapy: ACEi/ARB, diuretics, MRA as indicated.
- Anticoagulation: if atrial fibrillation present.
- Transplantation: end-stage cases with refractory HF or arrhythmias.
- 🔁 Lifelong cardiology follow-up in specialist inherited cardiac conditions clinic.
📚 References
- 2019 HRS Consensus on Arrhythmogenic Cardiomyopathy
- CSANZ Guidelines – Diagnosis & Management of ARVC
Cases - Arrhythmogenic Right Ventricular Cardiomyopathy (ARVC)
- Case 1 - Sudden Cardiac Symptoms in a Young Athlete: A 22-year-old semi-professional footballer collapses during training with palpitations and presyncope. ECG shows T-wave inversion in V1–V3 and episodes of ventricular tachycardia with left bundle branch block (LBBB) morphology. Echo and MRI demonstrate right ventricular dilation and regional wall motion abnormalities. Family history: cousin died suddenly at age 19. Diagnosis: ARVC presenting with exertional arrhythmia and risk of sudden cardiac death.
- Case 2 - Palpitations and Heart Failure in Middle Age: A 45-year-old man presents with progressive exertional dyspnoea, ankle swelling, and recurrent palpitations. ECG shows frequent ventricular ectopics. Cardiac MRI reveals fibro-fatty replacement of the right ventricular free wall with impaired systolic function. Genetic testing: plakophilin-2 mutation. Diagnosis: ARVC with arrhythmia and right-sided heart failure.
Teaching Commentary ❤️
ARVC is a rare inherited cardiomyopathy (often autosomal dominant, desmosomal gene mutations such as PKP2, DSG2, DSP) where fibro-fatty replacement of the right ventricular myocardium predisposes to ventricular arrhythmias, heart failure, and sudden cardiac death. Typical features: - Young adults, especially athletes. - ECG: T-wave inversion in V1–V3, epsilon waves, ventricular tachycardia with LBBB morphology. - Imaging: RV dilation/dyskinesia, fatty infiltration. Diagnosis uses the Task Force Criteria (structural, histological, ECG, arrhythmic, and family/genetic). Management: exercise restriction, implantable cardioverter-defibrillator (ICD) for sudden death prevention, anti-arrhythmics, and heart failure therapy if needed.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
