| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Dermatomyositis ✅
Related Subjects: |Relapsing Polychondritis |Reactive Arthritis |Raynaud's Phenomenon |Polymyositis |Dermatomyositis |Polyarteritis nodosa |Osteoporosis |Rheumatoid Arthritis |Systemic Sclerosis (Scleroderma) |Rheumatology Autoantibodies |Overlap Syndrome |Inclusion Body Myositis |Inflammatory Myopathies |Psoriatic Arthritis |Adult Onset Still's Disease |Alkaptonuria |Behcet's Syndrome
🌸 Dermatomyositis is an idiopathic inflammatory myopathy with characteristic cutaneous features and variable skeletal muscle involvement. Typical features include symmetrical proximal muscle weakness, a heliotrope rash (violaceous periorbital rash), and Gottron’s papules/sign over the MCP/PIP joints and extensor surfaces. ⚠️ In adult-onset disease, always think about associated malignancy, especially in higher-risk phenotypes.
🧬 About
- Immune-mediated inflammatory myopathy with prominent microangiopathy / vasculopathy, skin disease, and possible systemic involvement.
- May affect muscle, skin, lungs, swallowing, and occasionally the heart.
- Adult-onset dermatomyositis has a recognised association with occult malignancy; risk is highest around the time of disease onset.
📊 Epidemiology
- Rare condition; more common in women.
- Occurs in both children and adults.
- Adult-onset disease carries malignancy risk; juvenile dermatomyositis is not routinely associated with cancer.
🎗️ Malignancy Association
- Think particularly about malignancy in adult-onset disease, especially if there is older age at onset, male sex, dysphagia, cutaneous necrosis/ulceration, rapid onset, poor response to immunosuppression, or anti-TIF1-γ / anti-NXP2 positivity.
- Common associated cancers include lung, ovarian, breast, colorectal/gastrointestinal, and lymphoma.
- Nasopharyngeal carcinoma is particularly relevant in some East and South-East Asian populations.
- Continue routine age- and sex-appropriate national cancer screening as well as targeted assessment where indicated.
🩺 Clinical Features
- 💪 Symmetrical proximal muscle weakness – difficulty climbing stairs, rising from a chair, washing hair, or lifting arms overhead.
- 🌸 Skin signs:
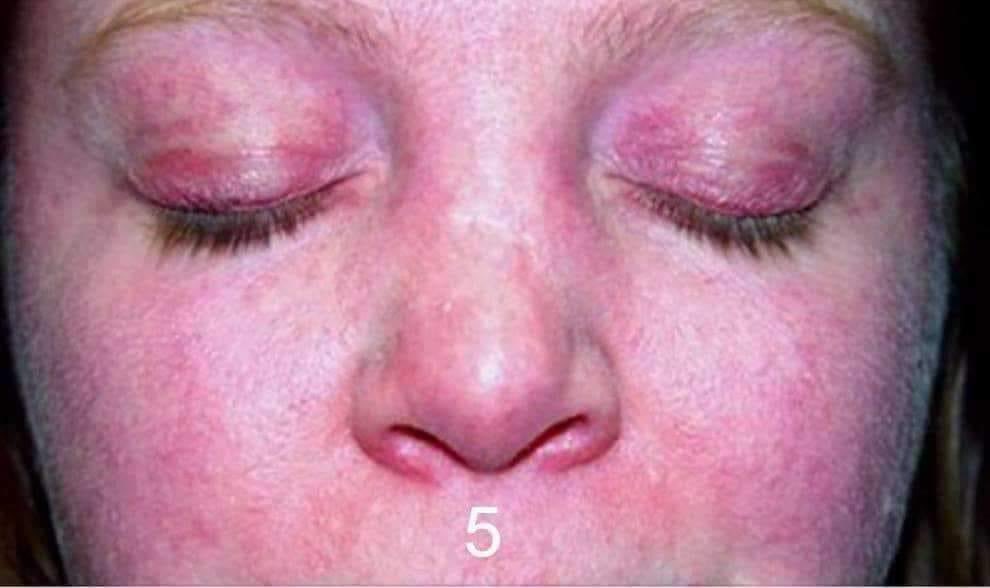
- Heliotrope rash with periorbital oedema.
- Gottron’s papules/sign over knuckles, elbows, or knees.
- Shawl sign / V-sign – photosensitive erythema over shoulders, upper chest, or back.
- Mechanic’s hands – hyperkeratotic, cracked fingertips (especially with antisynthetase overlap).
- Nailfold telangiectasia.
- Scalp erythema/pruritus may occur.
- 🫁 Lung involvement: interstitial lung disease, especially in antisynthetase or anti-MDA5 phenotypes.
- 🍽️ Dysphagia may occur and is clinically important because of weight loss and aspiration risk.
- ❤️ Occasionally associated with cardiac involvement.
- ⚖️ Constitutional features may include fatigue, weight loss, arthralgia, and reduced exercise tolerance.
🔬 Investigations
- Bloods: CK may be raised (but can be normal, especially in some phenotypes); also check AST/ALT, LDH, CRP/ESR, FBC, U&Es, LFTs, bone profile.
- Autoantibodies: request a myositis-specific / myositis-associated antibody panel.
- Anti-TIF1-γ, anti-NXP2 → malignancy risk markers in adult-onset disease.
- Anti-MDA5 → risk of rapidly progressive ILD.
- Anti-Mi-2 → classic cutaneous dermatomyositis phenotype.
- Anti-Jo-1 and other antisynthetase antibodies → antisynthetase syndrome / ILD / mechanic’s hands / Raynaud’s.
- MRI muscle: useful to identify inflamed muscle and guide biopsy.
- EMG: supports a myopathic process but is not diagnostic on its own.
- Muscle biopsy: classically shows perifascicular atrophy with perivascular/perimysial inflammation.
- Skin biopsy: may support the diagnosis where rash is prominent.
- Screen for ILD in higher-risk patients with chest imaging, pulmonary function tests (including gas transfer), and HRCT where indicated.
- Assess swallowing if dysphagia is suspected.
- Consider cardiac screening with ECG, echocardiography, and troponin I if clinically indicated.
- Malignancy screen: tailored to risk profile; in higher-risk adult patients consider CT thorax/abdomen/pelvis and further targeted tests as indicated.
💊 Management
- 🤝 Specialist MDT care – usually rheumatology ± neurology, dermatology, respiratory, SALT, physiotherapy, and oncology where needed.
- 📉 Glucocorticoids are usually first-line induction therapy.
- 🛡️ Add a steroid-sparing immunosuppressant early in many patients (for example methotrexate, azathioprine, mycophenolate, tacrolimus/ciclosporin depending on phenotype and organ involvement).
- 💉 Refractory / severe disease: consider IV methylprednisolone, IVIG, rituximab, or cyclophosphamide in specialist care.
- 🌞 Sun protection is important for cutaneous disease.
- 🏃 Exercise / rehabilitation with specialist physiotherapy or OT should be part of routine care.
- 🦴 Assess bone protection if prolonged steroids are used.
- 🍽️ Actively manage dysphagia, aspiration risk, nutrition, and respiratory complications.
🧾 Comparison of Inflammatory Myopathies
| Feature | 💉 Polymyositis* | 🌸 Dermatomyositis | 🧓 Inclusion Body Myositis |
|---|---|---|---|
| Typical age | Adults | Children or adults | > 50 years |
| Weakness pattern | Proximal | Proximal ± skin disease | Finger flexors + quadriceps, often asymmetric |
| Skin changes | No | Yes – heliotrope rash, Gottron’s papules/sign | No |
| CK | Usually raised | Usually raised, but may be normal | Normal or mildly raised |
| Cancer association | Less clear / lower than DM | Important association in adult-onset disease | Not a prominent classic association |
| Biopsy | Endomysial inflammation with CD8+ T cells | Perifascicular atrophy; perivascular/perimysial inflammation | Endomysial inflammation + rimmed vacuoles |
| Response to treatment | Variable | Often responsive to immunosuppression | Poor |
Teaching point 🩺: In adult-onset dermatomyositis, think in three parallel directions: muscle disease, skin disease, and systemic associations (especially malignancy, ILD, and dysphagia). Anti-Jo-1 is more suggestive of an antisynthetase phenotype than “classic dermatomyositis”, while anti-TIF1-γ and anti-NXP2 are more helpful when thinking about cancer risk.
*Pure polymyositis is now considered much less common than older textbooks suggested, and modern practice often reclassifies patients into other inflammatory myopathy subtypes.
:100%;">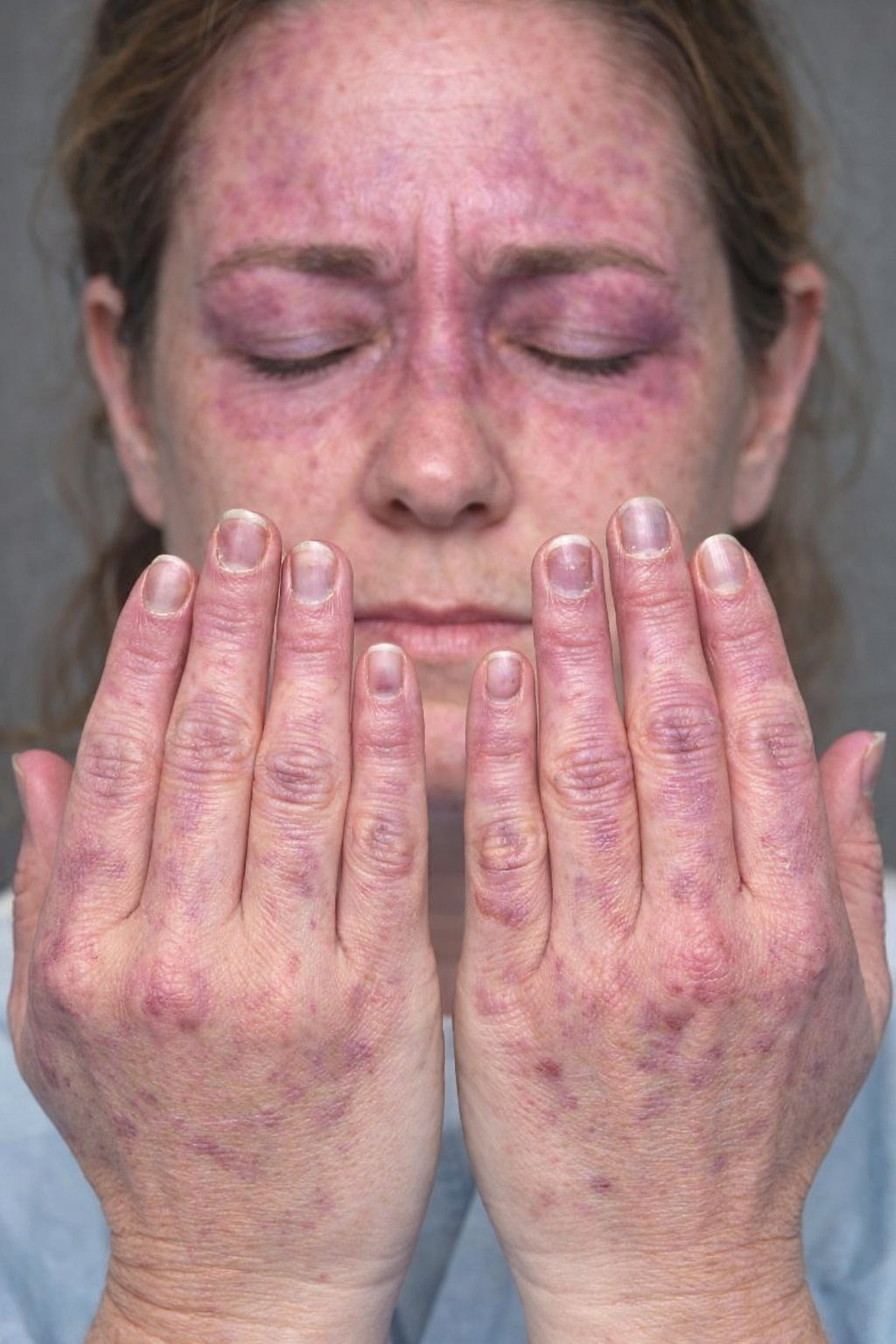
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
