| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Placental abruption
Related Subjects: |Antepartum haemorrhage |Postpartum haemorrhage |Acute Haemorrhage |Placenta praevia |Placenta abruption
⚠️ About
- Antepartum haemorrhage = any vaginal bleeding after 24 weeks gestation until delivery.
- Placental abruption = premature separation of the placenta from the uterine wall before birth.
- 🔑 It is a major cause of antepartum haemorrhage and a leading obstetric emergency.
- 🚨 Blood loss may be concealed (trapped behind placenta) → clinical severity can be underestimated.
📊 Aetiology
- Incidence ~1–2% of pregnancies.
- Bleeding occurs into the decidua basalis, shearing placenta away from uterus.
- Maternal uterine blood flow at term is 600–800 mL/min → risk of rapid, life-threatening haemorrhage.
⚠️ Risk Factors
- Pre-eclampsia / chronic hypertension
- Chorioamnionitis
- Cocaine use 🚬💉
- Polyhydramnios → sudden uterine decompression
- Trauma (RTC, falls, domestic violence)
- Smoking
- Male fetus
- Higher incidence in Black women
🩺 Clinical Features
- Vaginal bleeding (visible or concealed)
- Severe constant abdominal or back pain
- Uterus tense, tender, “woody” on palpation
- Uterine contractions or hypertonicity
- Fetal distress (abnormal CTG / absent FHR)
🔍 Differentials
- Placenta praevia
- Uterine rupture
- Appendicitis
- Chorioamnionitis
🖼️ Causes of Antepartum Haemorrhage
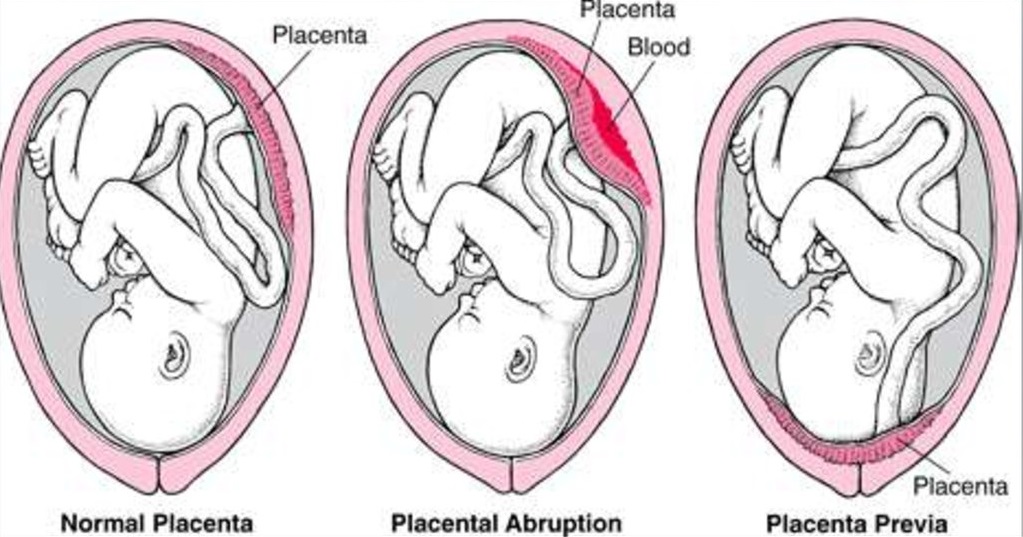
🧪 Investigations
- USS → poor sensitivity (only ~50% cases detected). Clinical diagnosis is key.
- Bloods: FBC, coagulation screen, fibrinogen (↓ early in DIC), U&E, cross-match 4–6 units.
- CTG for continuous fetal monitoring.
🏥 Management
- Stabilise mother first: large-bore IV access, IV fluids, cross-match, blood products as needed.
- Fetal viability: assess viability and CTG trace.
- Steroids: if preterm, give corticosteroids for lung maturity.
- Monitor for DIC: keep close watch on coagulation profile.
- Delivery:
- Vaginal delivery possible if mother/fetus stable.
- 🚨 Emergency C-section if heavy bleeding or fetal distress.
⚠️ Complications
- Maternal: haemorrhagic shock, DIC, ATN (renal injury), Couvelaire uterus (blood infiltration → uterine atony)
- Fetal: intrauterine death, prematurity, hypoxia
📌 Exam Pearls
- Visible PV loss ≠ severity → concealed haemorrhage may be massive.
- Tense, woody uterus + constant pain = classic sign.
- Placental abruption vs praevia → painful bleeding vs painless bleeding.
- Always stabilise mother before focusing on fetus.
- DIC risk is high → always monitor clotting + fibrinogen.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
