| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Air Embolism ✅
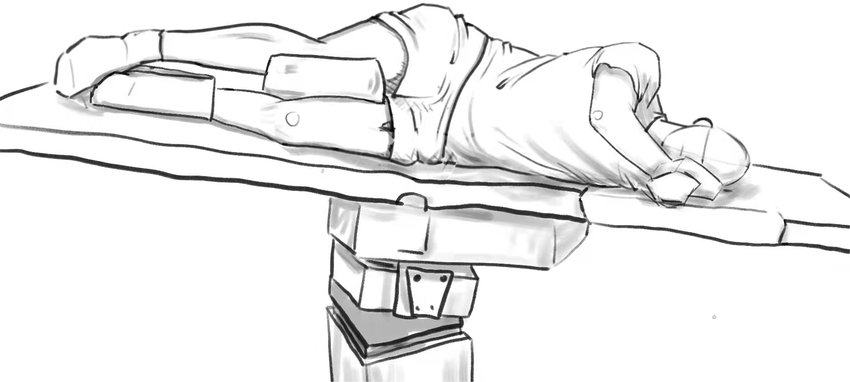
💨 Air Embolism occurs when air bubbles enter the bloodstream, obstructing circulation. This can happen during surgery, trauma, medical procedures, or diving accidents 🏊♂️. Severity depends on volume of air and site of obstruction. Clinical features include acute neurological deficits (e.g., hemiparesis, seizures), cardiovascular collapse, and hypoxia. 📌 Immediate Positioning: Left lateral decubitus + Trendelenburg (head down, left side down) → traps air in the right ventricular apex, slowing systemic entry. Give high-flow oxygen: 10–15 L/min via non-rebreather mask or up to 60 L/min via high-flow nasal cannula.
📌 About
- ⚙️ Mechanism: Air enters venous or arterial circulation → obstructs blood flow → impaired perfusion.
- 🫀 Venous Air Embolism (VAE): Air reaches right heart → pulmonary artery obstruction → hypoxia, RV strain, cardiovascular collapse.
- 🧠 Arterial Air Embolism (AAE): Can reach brain, heart, kidneys → stroke, MI, multiorgan injury.
- 🤿 Diving/Decompression: Rapid ascent → nitrogen bubbles mimic air embolism (decompression sickness).
- ⚠️ Severity: Small volumes (0.5–1 mL in coronary/cerebral arteries) can be fatal; >50 mL venous air may cause cardiovascular collapse.
🔬 Pathophysiology
- 🩸 Venous entry favoured when site is above right atrium → negative pressure sucks in air.
- 🚪 Arterial embolism may arise via pulmonary barotrauma or paradoxical embolism through PFO/ASD.
- 🧠 Cerebral & coronary arteries most vulnerable → stroke-like deficits, MI.
📋 Causes
- 🩻 Surgical: Neurosurgery, cardiothoracic surgery, central line insertion/removal.
- 🪓 Trauma: Penetrating chest/neck injuries or fractured veins.
- 💉 Central Lines & Catheters: Most common iatrogenic cause.
- 🤿 Diving Accidents: Poor decompression control → overlap with nitrogen embolism.
- 💨 Positive Pressure Ventilation: Barotrauma → alveolar-vascular air entry.
🩺 Clinical Features / Red Flags
- 😮 Dyspnoea, hypoxia, cyanosis
- ❤️ Chest pain, arrhythmias
- 🧠 Neurological: dizziness, seizures, confusion, focal deficits, hemiparesis
- 📉 Hypotension, obstructive shock
- 💔 Cardiac arrest in severe cases
🔎 Investigations
- 🧪 ABG → hypoxia ± metabolic acidosis
- 📈 ECG → RV strain, tachycardia, ST changes
- 🩻 CXR → non-specific, may show pulmonary oligemia
- 🫀 TEE → sensitive for air bubbles in RA/RV (especially intraoperative)
- 🧪 Consider blood tests to rule out alternative causes (e.g., PE, stroke)
🩺 Differentials
- 🫁 Pulmonary embolism
- 🧠 Stroke / TIA
- ❤️ Myocardial infarction
- 🫁 Tension pneumothorax
- 💔 Cardiac tamponade
🚨 Complications
- 💔 Cardiac arrest / obstructive shock
- ❤️ Myocardial infarction
- 🧠 Hypoxic brain injury / stroke
- 🫁 ARDS & respiratory failure
🛡️ Prevention
- 🏥 Careful central line insertion/removal; use air filters where possible
- 🤿 Divers → controlled ascent, decompression stops
- 💉 Maintain air-tight connections, patient positioning during line manipulation
⚕️ Management
- 🔄 Resuscitation: ABCs, high-flow oxygen (10–15 L/min NRB or 60 L/min HFNC)
- 🛏️ Position: Left lateral decubitus + Trendelenburg
- 🤐 Intubation/ventilation if severe hypoxia
- 💧 Fluids ± inotropes to maintain preload & cardiac output
- 💉 Aspiration via central line if RA accessible (intraoperative / ICU setting)
- 🌊 Hyperbaric Oxygen Therapy (HBOT) → gold standard for cerebral or cardiac involvement; ideally <8 hours from onset
- 🔪 Open chest aspiration → rare, intraoperative emergency
💡 Teaching Pearl: Early recognition + positioning + high-flow oxygen can reverse neurological deficits and prevent mortality. Neurological recovery may be slow but often improves with prompt intervention.
📉 Prognosis
- ⏱️ Dependent on speed of recognition and treatment
- ✅ Early intervention → good functional recovery
- ❌ Delay → permanent neurological injury or death
📚 References
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
