| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Trauma: Cardiac Arrest
Related Subjects: |Initial Trauma Assessment and Management |Thoracic Trauma Assessment and Management |Flail Chest Rib fractures |Resuscitative Thoracotomy |Haemorrhage control |Traumatic Head/Brain Injury |Traumatic Cardiac Arrest |Abdominal trauma |Tranexamic Acid |Silver Trauma |Cauda Equina |Spinal Cord Anatomy |Initial Trauma Assessment and Management |Cervical Spine Immobilization and Management |Anatomy of the Cervical Vertebrae C1 (Atlas) and C2 (Axis) |Trauma: Spinal Injury |Adult Resus:Basic Life Support |Adult Resus: Advanced Life Support |Resus:Acute Haemorrhage
Introduction
🚨 Trauma-related cardiac arrest (TRCA) is a critical emergency where the heart stops effectively due to severe injury. Unlike medical cardiac arrest, TRCA usually has reversible mechanical or physiological causes (bleeding, hypoxia, tamponade) and requires a targeted trauma approach rather than standard ACLS.
Causes
- 🩸 Hypovolemia: severe internal/external haemorrhage.
- 🫁 Tension pneumothorax: lung collapse with mediastinal shift.
- 💔 Cardiac tamponade: pericardial blood/fluid compressing the heart.
- 🌬️ Hypoxia: airway obstruction or respiratory failure.
- 🫀 Massive PE: rare but possible after trauma.
- ❄️ Hypothermia: low core temperature impairs contractility.
Pathophysiology
Most TRCAs stem from 🩸 haemorrhagic shock → preload failure → PEA. Obstructive causes (tamponade, tension pneumothorax) prevent filling. 🌬️ Hypoxia worsens cellular dysfunction, precipitating arrest.
Assessment (ATLS framework)
- 🅰️ Airway: patency, C-spine control.
- 🅱️ Breathing: chest movement, auscultation, needle decompression if suspected tension.
- 🅲️ Circulation: pulses, haemorrhage control, IV/IO access.
- 🅳️ Disability: GCS, pupillary response.
- 🅴 Exposure: identify injuries, prevent hypothermia.
Management Principles
🏥 Key difference from medical arrest: Fix the cause (bleeding, tamponade, pneumothorax) rather than prolonged CPR + drugs. Chest compressions are adjunctive, not definitive.
Immediate Actions
- ⚠️ Scene safety and activate trauma team.
- 🤝 Call surgical/cardiothoracic backup early.
- 💨 Airway: intubate if indicated, give 100% O₂.
- ❤️ Start compressions only if no cardiac output.
- 🔎 Use POCUS/eFAST to check cardiac activity, tamponade, pneumothorax, bleeding.
Treating Reversible Causes
- 🩸 Hypovolemia: direct pressure/tourniquets, pelvic binder, TXA, MHP (1:1:1 RBC:plasma:platelets).
- 🫁 Tension pneumothorax: needle decompression ➝ chest tube.
- 💔 Tamponade: pericardiocentesis (temporary) ➝ resuscitative thoracotomy.
- 🌬️ Hypoxia: airway clearance, intubation, ventilation.
- ❄️ Hypothermia: warm blankets, warmed IV fluids, heated oxygen.
Adjuncts
- 🖥️ Ultrasound: assess cardiac motion (if none, prognosis poor).
- ⚡ Defibrillate if VF/VT present (rare in TRCA).
- 💊 Drugs: limited role-focus on surgical/trauma fixes.
Special Considerations
- 🔪 Resuscitative Thoracotomy: Indicated for penetrating thoracic trauma with signs of life in ED. Allows tamponade release, cardiac massage, aortic cross-clamp.
- ⏹️ Termination: Blunt trauma arrest without signs of life and no ROSC after reversible causes addressed → cease efforts (per ERC/RCEM guidance).
Prognosis
📉 Overall survival is < 5%. 🔪 Penetrating trauma (esp. cardiac stab wounds) → best outcomes. 🚗 Blunt trauma arrest → survival is extremely rare.
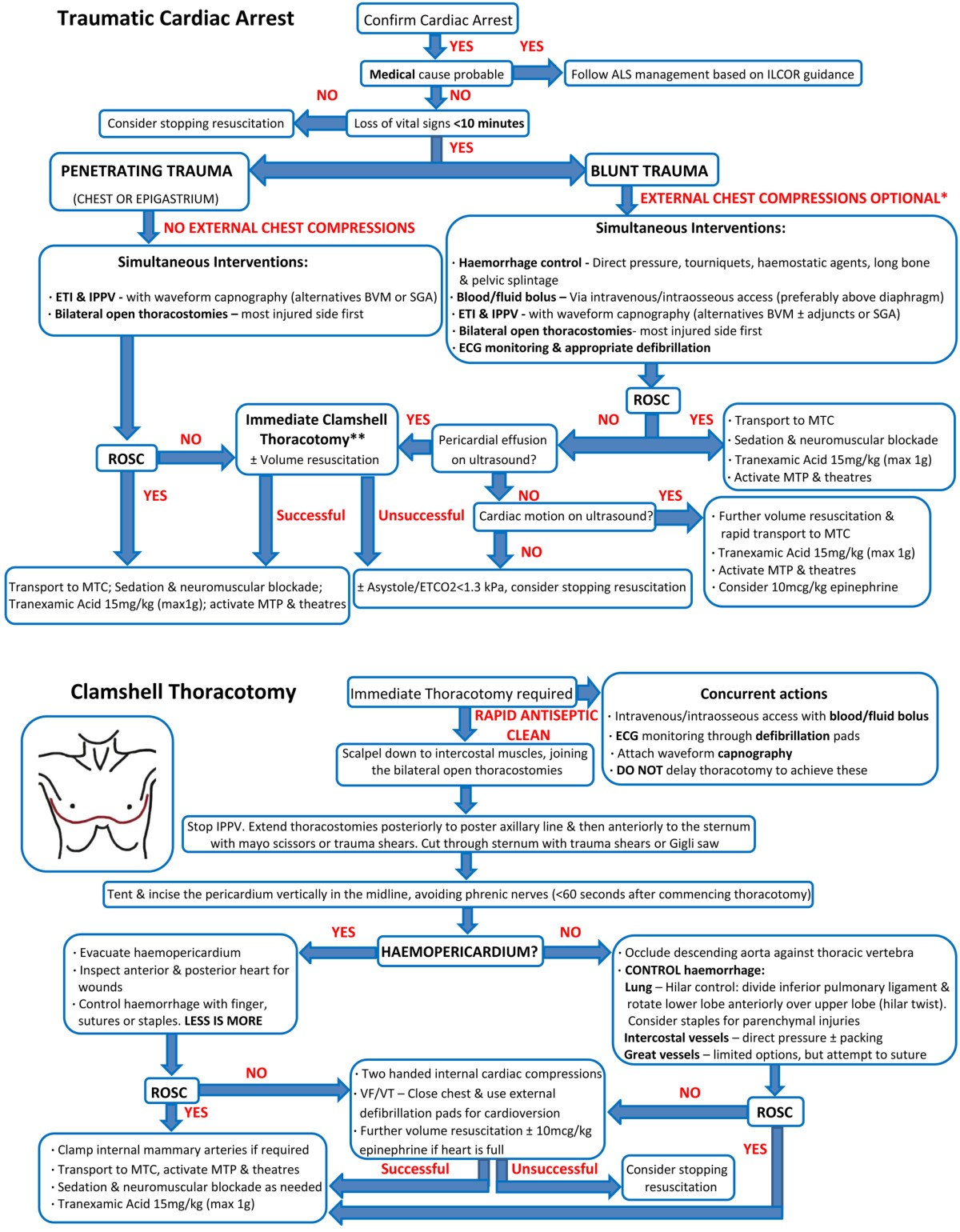
Conclusion
TRCA requires rapid recognition and immediate treatment of reversible causes. 💡 Unlike medical cardiac arrest, the emphasis is surgical: haemorrhage control, decompression, thoracotomy. Outcome depends on mechanism-penetrating > blunt.
References
- ATLS 10th Ed. American College of Surgeons, 2018.
- Soar J, Nolan JP, Böttiger BW, et al. ERC Guidelines, 2021.
- Hopson LR, Hirsh E, Delgado J, et al. J Am Coll Surg 2003;196(1):106-112.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
