Related Subjects:Acute Cholecystitis
|Acute Appendicitis
|Chronic Peritonitis
|Abdominal Aortic Aneurysm
|Ectopic Pregnancy
|Acute Cholangitis
|Acute Abdominal Pain/Peritonitis
|Assessing Abdominal Pain
|Penetrating Abdominal Trauma
|Acute Pancreatitis
|Acute Diverticulitis
⚠️ Pain may be absent or muted in certain high-risk groups - elderly patients, those on long-term steroids, diabetics, and the very frail. Always think: is the patient moribund/in extremis?
If so → follow ABC, call for senior/surgical help early, gain IV access, give oxygen, start IV crystalloids, provide analgesia, and send urgent bloods (including lactate, FBC, U&E, amylase, and cross-match if haemorrhage is suspected).
👉 If shocked with bleeding → get 2 wide-bore lines, activate major haemorrhage protocol, consider urgent O negative blood.
👉 If septic → IV antibiotics + fluids without delay.
| 🚑 Acute Abdominal Pain – Emergency Management Summary |
|---|
- 🔴 ABCDE + NEWS, Nil by mouth, early senior review
- 🩻 Initial investigations: Erect CXR / AXR, ECG, FBC/U&E/CRP/Lactate
- 💉 Get 2 large-bore IV lines, send bloods, start IV fluids ± antibiotics
- ⚠️ Red flags: high NEWS, peritonism (silent/rigid abdomen), haemodynamic instability → escalate immediately
- Special diagnostic triggers:
- Abdominal pain + low BP → think sepsis
- Abdominal pain + low BP + >50 yrs → leaking AAA
- Abdominal pain + fertile female → ectopic pregnancy
- Abdominal pain + AF/MI → ischaemic bowel
- Abdominal pain + gallstones/alcohol → pancreatitis
|
📖 Acute Abdomen – Key Principles
- Sudden onset severe abdominal pain (<24h) → always assume potentially lethal pathology until proven otherwise
- Expert assessment + early surgical involvement crucial
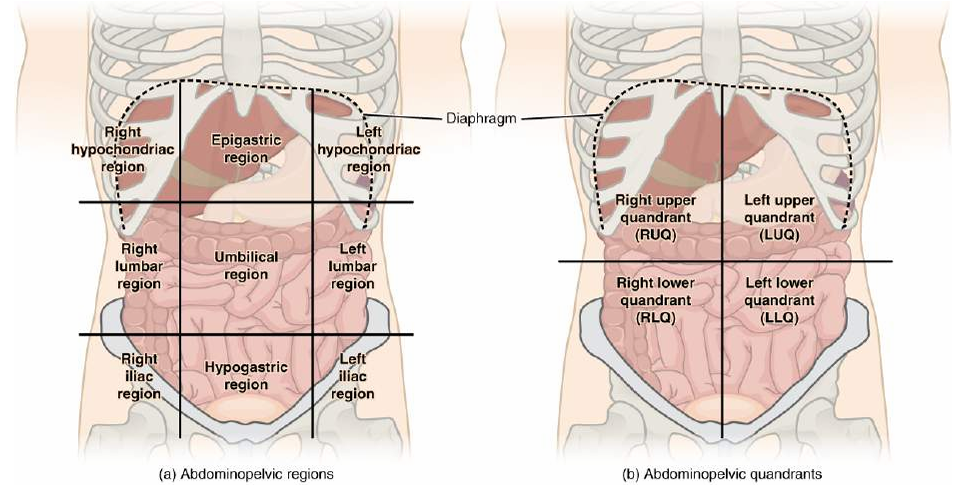
- Pain localisation often follows embryological origin:
- 🌐 Foregut → Epigastrium
- 🌐 Midgut → Peri-umbilical
- 🌐 Hindgut → Below umbilicus
🧠 Pathophysiological Background
- Parietal peritoneum richly innervated → inflammation causes localised pain, guarding & rigidity
- Visceral pain → poorly localised, dull (e.g. appendicitis starts peri-umbilical)
- When parietal peritoneum becomes involved → pain localises (e.g. appendicitis to RIF at McBurney’s point)
- Always examine hernial orifices to exclude strangulated hernia
🔎 Common Causes of Acute Abdominal Pain
| Cause |
Clinical Features |
Diagnostic Tests |
Management |
| Appendicitis |
RIF pain, anorexia, fever, rebound tenderness |
FBC, US/CT |
Appendicectomy ± antibiotics |
| Cholecystitis |
RUQ pain, post-prandial, fever |
US, LFTs |
Cholecystectomy |
| Pancreatitis |
Epigastric pain radiating to back, vomiting |
Amylase/lipase, CT |
IV fluids, analgesia, NBM |
| Ectopic Pregnancy |
Lower pain, bleeding, missed period |
hCG, TV ultrasound |
Methotrexate or surgery |
| AAA (ruptured) |
Shock, back/abdo pain, pulsatile mass |
Bedside US, CT angio |
Resuscitation + vascular surgery |
🧾 Additional Diagnostic Pearls
- 📉 Silent abdomen + rigidity → peritonitis → surgical emergency
- 🧪 Amylase 3× ULN → pancreatitis (but can rise in perforation, ectopic, DKA)
- 📍 Pain radiation clues:
- Shoulder → diaphragmatic irritation
- Back → AAA or pancreatitis
- Periumbilical → appendicitis (early)
- 🚺 All women of child-bearing age → pregnancy test mandatory
🧰 Investigations
- Bloods: FBC, U&E, CRP, LFTs, Ca, glucose, amylase/lipase, group & save
- Urine dip ± culture; urine pregnancy test
- ECG – exclude ACS
- Imaging: AXR (limited), CXR (free air, pneumonia), CT abdo (most useful), USS (biliary/gyne)
- Blood cultures if sepsis suspected
- Special: CT angiography (mesenteric ischaemia), porphobilinogen (acute porphyria)
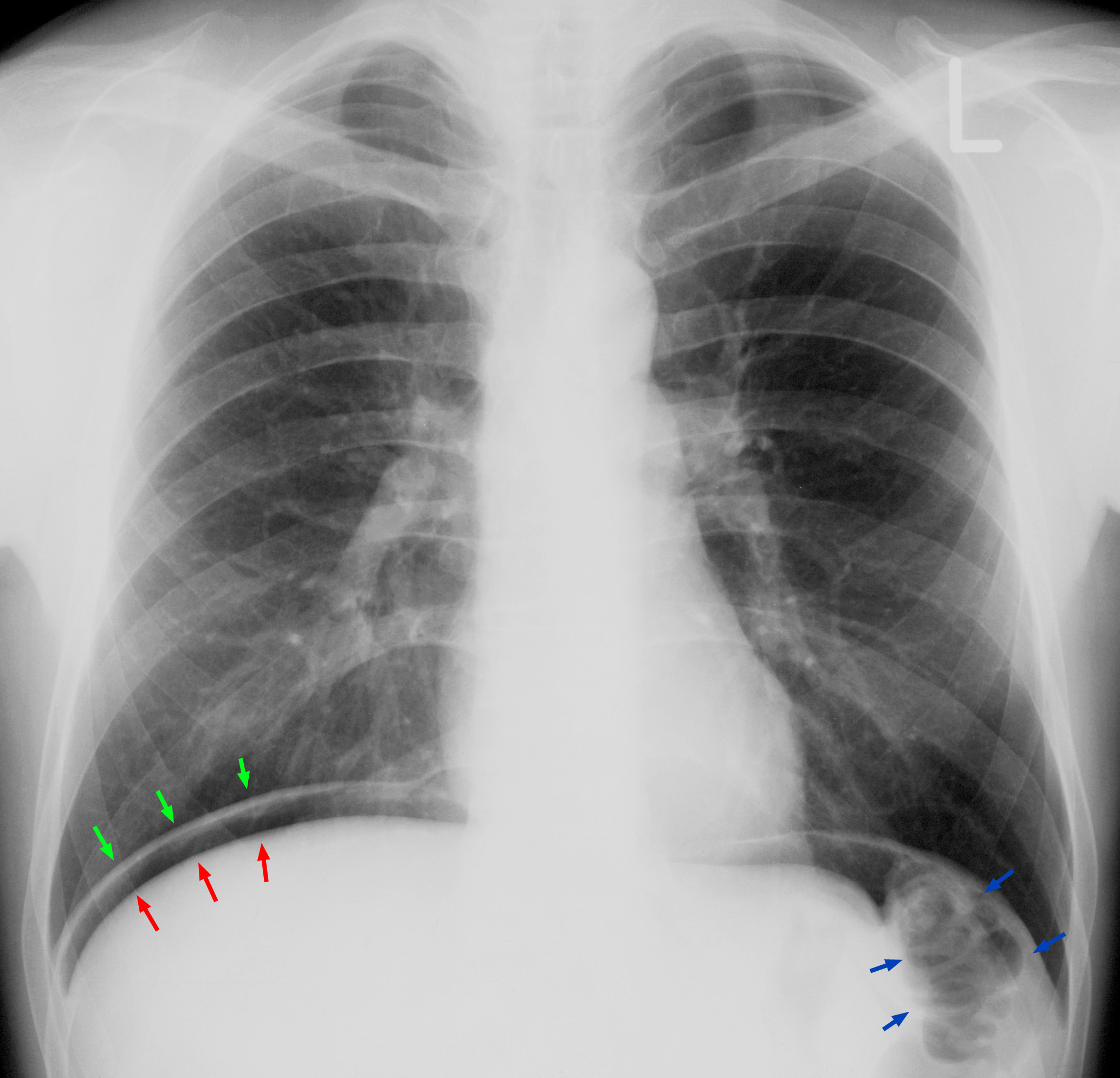
🫁 Causes of Free Sub-diaphragmatic Gas on AXR
- Perforated viscus (peptic ulcer, diverticulitis, appendix)
- Gas-forming infection
- Iatrogenic (post-laparoscopy)
- Pleuroperitoneal fistula
 ⚡ Acute Management – Principles
⚡ Acute Management – Principles
- Stabilise → ABC, O2, IV access, fluids, catheter, NG tube if obstruction
- 3L/day crystalloids minimum in pancreatitis/obstruction
- Correct electrolytes, insulin infusion if DKA
- Early antibiotics if sepsis or perforation suspected
- Urgent senior surgical review
- CT abdo for diagnosis, laparotomy if peritonitis/rupture
- DVT prophylaxis unless contraindicated
🔪 Surgical Management
- Do not delay surgery except for resuscitation
- Broad-spectrum IV antibiotics (e.g. Tazocin ± Gentamicin ± Metronidazole)
- Remove infarcted/perforated tissue
- Repair perforations, drain abscesses, lavage peritoneum
- Massive haemorrhage protocol if bleeding

 ⚡ Acute Management – Principles
⚡ Acute Management – Principles
